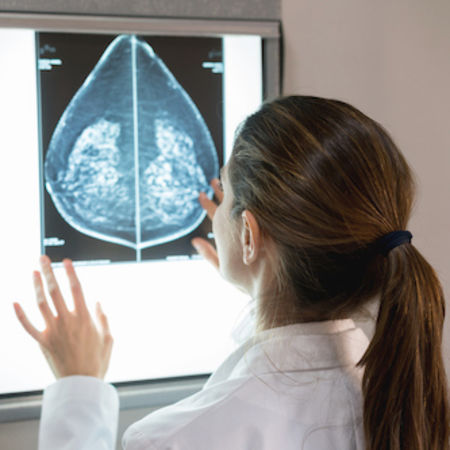
Approximately 50% of women in the United States between the ages of 40 to 74 years old have dense breasts (an estimated 27.6 million women). The recent widespread inclusion of breast density information into screening mammography reports in 36 US states and suggestion to consider supplemental imaging has resulted in creating awareness and leading women to raise questions about breast density and supplemental imaging with their doctors. Clinicians need to be knowledgeable, therefore, of the clinical significance of breast density and how it may be useful when combined with breast cancer risk to inform screening discussions.
Breast density, a term in radiology which describes the proportion of parenchymal relative to fatty tissue in mammograms, is a strong and prevalent risk factor. With increasing breast density, the risk of having a breast cancer masked or hidden on mammography increases, as does future breast cancer risk.
You may also like: U.S. dense breast notification laws: awareness & early cancer detection after mammo
In clinical practice, breast density is assigned by radiologists into one of 4 breast imaging reporting and data system (BI-RADS) categories: almost entirely fatty, scattered areas of fibroglandular density, heterogeneously dense, or extremely dense. The first 2 categories are considered nondense and the last 2 are considered dense. Clinical BI-RADS density assessment is subjective, with interrater and intrarater reliability resulting in moderate to substantial agreement. Commercial software is available to provide automated BI-RADS and quantitative volumetric density estimates on digital mammography. Automated measures are more reproducible than clinical BI-RADS density classification on repeated examinations and similarly predict overall invasive and interval cancer risk (ie, risk of being diagnosed with invasive breast cancer within 1 year of negative screening mammography result).
Breast density has been incorporated into breast cancer risk prediction models to estimate future breast cancer risk because models with a measure of breast density show better discrimination than models with clinical factors only. The Breast Cancer Surveillance Consortium (BCSC) risk model was developed in US women undergoing mammography, incorporates BI-RADS breast density,3 has accurate calibration, predicts 5- and 10-year invasive cancer risk in the most prevalent racial/ethnic groups in the United States, and has been externally validated in 2 different mammography cohorts.4 The Tyer-Cuzick model was developed based on white women in the United Kingdom to calculate 10-year invasive cancer risk and incorporates qualitative or quantitative density measures, but is less well calibrated for US women undergoing mammography.5 The Breast and Ovarian Analysis of Disease Incidence and Carrier Estimation Algorithm is a genetic-based risk model that incorporates BI-RADS density measures and predicts 10-year invasive cancer risk.6
Breast density has also been used to stratify women’s interval cancer risk. More than half (64%) of the cases of interval cancer diagnosed following routine digital screening mammography occur in women with dense breasts; however, only 24% of the women with dense breasts who also have higher than average breast cancer risk (BCSC 5-year risk ≥1.67%) are at high risk of an interval cancer (>1 interval cancer/1000 mammograms).1 Women with dense breasts and a BCSC 5-year risk of 2.5% or higher (21% of women with dense breasts) are at greatest risk of interval stage IIb or higher breast cancer. Thus, knowing a woman’s breast density and breast cancer risk informs the likelihood that breast cancer will be missed on mammography and identifies subgroups of women who have the most potential to benefit from supplemental imaging.
Recommendations for how dense breasts should be managed in clinical practice vary from stating that there is insufficient evidence on whether supplemental imaging is effective to recommending the consideration of supplemental ultrasonography (Supplement). Studies of the effectiveness of supplemental imaging in women with dense breasts have primarily been observational, have not incorporated a formal risk assessment, and have often included women with a personal history of breast cancer.
Supplemental imaging studies provide evidence of an incremental increase in breast cancer detection and benign breast biopsy results compared with screening with only digital mammography (Supplement). Breast magnetic resonance (MR) imaging and molecular breast imaging tests have the highest incremental cancer and occult cancer detection rates but are expensive and invasive relative to supplemental ultrasonography and digital breast tomosynthesis (DBT).
Two randomized clinical trials have demonstrated a significant reduction in interval breast cancer rates with supplemental imaging. The Japan Strategic Anti-cancer Randomized Trial reported fewer cases of interval breast cancer with annual supplemental ultrasonography plus mammography vs mammography alone in average-risk women aged 40 to 49 years, but more benign biopsies in the supplemental imaging group. The Dense Tissue and Early Breast Neoplasm Screening trial reported fewer cases of interval breast cancer with biennial supplemental MR imaging plus mammography vs mammography alone in women aged 50 to 74 years with extremely dense breasts. Studies have not evaluated whether supplemental imaging reduces advanced breast cancer rates or breast cancer mortality.
To date, no published randomized clinical trials have evaluated the comparative effectiveness of different screening intervals according to the extent of breast density. However, modeling and cohort studies have evaluated the association between breast density and long-term screening outcomes (eg, deaths averted or reduction in advanced breast cancer) by different screening intervals.
One study used 3 validated microsimulation models to estimate breast cancer deaths averted based on breast density combined with other risk factors among women aged 50 to 74 years.9 This study found that women with dense breasts and no more than 1 weak risk factor (relative risk factor level 1.3; eg, 1 first-degree relative with breast cancer) screened annually vs biennially had slightly more deaths averted (lifetime benefit is estimated at approximately 2 per 1000 women), but 50% additional benign breast biopsies and 40% to 48% additional overdiagnosis cases.
The largest number of deaths averted were in women who undergo annual screening with very strong risk factors (relative risk factor level 4.0; eg, atypical ductal hyperplasia) at any level of breast density or with strong risk factors (relative risk factor level 2.0; eg, 2 first-degree relatives with breast cancer) and dense breasts, such that annual screening in these groups is cost effective. A large cohort study examined the proportion of advanced breast cancers by screening mammography frequency according to breast density and found the proportion of tumors that were stage IIb or higher was greater for biennial than annual screeners for women aged 40 to 49 years with extremely dense breasts, but not for women aged 50 to 74 years with heterogeneously or extremely dense breasts.10 Women who underwent annual screening in both age groups had almost a 2-fold higher cumulative 10-year risk of benign biopsy results. These studies suggest a combined breast density/risk-based approach to tailoring screening interval allows for informing the balance of screening benefits and harms.
DBT is a newer breast screening modality that has a lower recall rate and slightly higher cancer detection rate than digital mammography (Supplement). However, no published evidence indicates that interval cancer rates differ for digital vs DBT mammography in women with dense breasts. Thus, whether women are undergoing digital or DBT mammography, breast density and breast cancer risk should be considered because the combined effect of these factors informs interval cancer risk and long-term screening benefits and harms.
Women aged 50 to 74 years undergoing screening mammography should be informed of their clinical or automated BI-RADS breast density in combination with their overall breast cancer risk to determine if they have dense breasts and low breast cancer risk and can consider routine biennial screening. Conversely, women with dense breasts and high breast cancer risk due to strong risk factors or with dense or nondense breasts and very strong risk factors may want to consider annual screening, supplemental imaging, or both to reduce interval or advanced breast cancer risk because modeling studies suggest annual screening averts substantially more deaths from breast cancer than biennial screening.
Although screening guidelines are variable for average-risk women aged 40 to 49 years, women with a first-degree relative with breast cancer or a history of benign breast biopsy results may want to consider an initial mammogram to learn of their breast density because having dense breasts combined with other risk factors may put them at high enough risk to consider routine screening.
Annual screening with digital or DBT mammography, supplemental imaging, or both of all women with dense breasts without considering overall breast cancer risk could result in more harm than good with increasing risk of anxiety, benign breast biopsies, and overdiagnosis.
Women and health care professionals should discuss breast density in the context of breast cancer risk so women can decide if their risk is high enough that the potential benefits of annual screening mammography and/or supplemental imaging are likely to outweigh the potential harms or that their risk is low to average and that more frequent screening and supplemental imaging will lead to more frequent harms with only a small additional chance of benefit.
Source: JAMA
Image credit: iStock
References:
Latest Articles
Radiology, breast cancer, JAMA, mammogram, breast screening, dense breast
Breast density, a radiologic term that describes the proportion of parenchymal relative to fatty tissue in mammograms, is a strong and prevalent risk factor. With increasing breast density, the risk of having a breast cancer masked or hidden on mammograph