A new MRI study published in the journal Radiology has found distinct injury patterns in the brains of people with concussion-related depression and anxiety. The findings may open the door to improved treatment and understanding of these common disorders, according to researchers.
Understanding what triggers psychiatric disorders like depression, anxiety and irritability following concussion — also known as mild traumatic brain injury — is rather difficult since conventional MRI results in most of these patients are normal. Hence, for this study, researchers from the University of Pittsburgh Medical Center (UPMC) used a special MRI technique called diffusion tensor imaging (DTI) that measures the integrity of white matter — the brain’s signal-transmitting nerve fibres.
The UPMC team examined whether injuries to the nerves may be the root cause of these post-traumatic depression and anxiety symptoms. They obtained DTI and neurocognitive testing results for 45 post-concussion patients, including 38 with irritability, 32 with depression and 18 with anxiety. These data were compared with those of 29 post-concussion patients who had no neuropsychiatric symptoms.
The results revealed unique white matter injury patterns in the patients who had depression or anxiety. Compared to controls, patients with depression had decreased fractional anisotropy (FA), a measure of the structural integrity of white matter connections, around an area near the deep grey matter of the brain that is strongly associated with the brain’s reward circuit.
“The regions injured in concussion patients with depression were very similar to those of people with non-traumatic major depression disorder,” notes lead author Lea M. Alhilali, MD, assistant professor of radiology at UPMC. “This suggests there may be similar mechanisms to non-trauma and trauma-dependent depression that may help guide treatment.”
Anxiety patients had diminished FA in a part of the brain called the vermis that helps modulate fear-related behaviours. Since the vermis has not been associated with dysfunction in non-traumatic anxiety disorders, this finding may indicate that different treatment targets are required for patients with anxiety after trauma, the UPMC researchers say.
No regions of significantly decreased FA were seen in patients with irritability relative to the control subjects.
Dr. Alhilali cites two major implications for this study. "First, it gives us insight into how abnormalities in the brain occur after trauma, and second, it shows that treatments for non-trauma patients with neuropsychological symptoms may be applicable to some concussion patients,” she says.
Her team hopes to take this research further by comparing DTI findings in concussion patients with depression to those of people who have non-trauma-related depressive disorders.
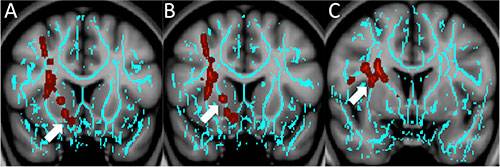
Figure 1. Coronal images derived from tract-based spatial statistics results and rendered on T1-weighted MR images from the Montreal Neurological Institute atlas show how patients with depression have significantly decreased fractional anisotropy in the region of A, the right nucleus accumbens (arrow) or “reward centre,” as well as B, the anterior limb of the internal capsule (arrow) and C, the superior longitudinal fasciculus (arrow) — regions that are involved in depressive disorders in non-traumatic and traumatic settings.
Source and image credit: RSNA
Understanding what triggers psychiatric disorders like depression, anxiety and irritability following concussion — also known as mild traumatic brain injury — is rather difficult since conventional MRI results in most of these patients are normal. Hence, for this study, researchers from the University of Pittsburgh Medical Center (UPMC) used a special MRI technique called diffusion tensor imaging (DTI) that measures the integrity of white matter — the brain’s signal-transmitting nerve fibres.
The UPMC team examined whether injuries to the nerves may be the root cause of these post-traumatic depression and anxiety symptoms. They obtained DTI and neurocognitive testing results for 45 post-concussion patients, including 38 with irritability, 32 with depression and 18 with anxiety. These data were compared with those of 29 post-concussion patients who had no neuropsychiatric symptoms.
The results revealed unique white matter injury patterns in the patients who had depression or anxiety. Compared to controls, patients with depression had decreased fractional anisotropy (FA), a measure of the structural integrity of white matter connections, around an area near the deep grey matter of the brain that is strongly associated with the brain’s reward circuit.
“The regions injured in concussion patients with depression were very similar to those of people with non-traumatic major depression disorder,” notes lead author Lea M. Alhilali, MD, assistant professor of radiology at UPMC. “This suggests there may be similar mechanisms to non-trauma and trauma-dependent depression that may help guide treatment.”
Anxiety patients had diminished FA in a part of the brain called the vermis that helps modulate fear-related behaviours. Since the vermis has not been associated with dysfunction in non-traumatic anxiety disorders, this finding may indicate that different treatment targets are required for patients with anxiety after trauma, the UPMC researchers say.
No regions of significantly decreased FA were seen in patients with irritability relative to the control subjects.
Dr. Alhilali cites two major implications for this study. "First, it gives us insight into how abnormalities in the brain occur after trauma, and second, it shows that treatments for non-trauma patients with neuropsychological symptoms may be applicable to some concussion patients,” she says.
Her team hopes to take this research further by comparing DTI findings in concussion patients with depression to those of people who have non-trauma-related depressive disorders.
* * * * * * * * * * * *
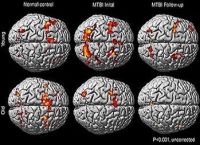
Top image. A, Axial and B, sagittal images derived from tract-based spatial statistics (TBSS) results and rendered on T1-weighted MR images from the Montreal Neurological Institute atlas indicate that significant white matter differences in patients with mTBI and anxiety involve the cerebellar vermis, the region responsible for fear conditioning. Voxels with significant differences detected with TBSS were thickened by using the TBSS fill function into local tracts (red) and overlaid on the white matter skeleton (blue). 
Figure 1. Coronal images derived from tract-based spatial statistics results and rendered on T1-weighted MR images from the Montreal Neurological Institute atlas show how patients with depression have significantly decreased fractional anisotropy in the region of A, the right nucleus accumbens (arrow) or “reward centre,” as well as B, the anterior limb of the internal capsule (arrow) and C, the superior longitudinal fasciculus (arrow) — regions that are involved in depressive disorders in non-traumatic and traumatic settings.
Source and image credit: RSNA
Latest Articles
healthmanagement, trauma, brain injury, depression, anxiety, diffusion tensor imaging
A new MRI study published in the journal Radiology has found distinct injury patterns in the brains of people with concussion-related depression and anxiety.