ICU Management & Practice, Volume 21 - Issue 2, 2021
This article highlights the key points that fall under the meaning of humanisation
as part of the ICU Liberation bundle.
Introduction
How would a patient describe their stay inside an Intensive Care Unit (ICU)? Would it be cold, lonely, a place full of uncertainty? Painful, uncomfortable or scary? The length of stay (LOS) in the ICU may be the most traumatic experience a person can endure. A duel between life and death. A change in hospital infrastructure, an organised multidisciplinary team, humanised centred interventions and modified strategies to obtain higher functionality levels can have a huge impact not only on the patient but on their families as well. The ABCDEF + GH bundle represents an evidence-based guide for clinicians to approach the organisational changes needed for optimising ICU patient recovery and outcomes. Humanisation (H) may be the last letter in the bundle, but that does not make it the least important. The central aspect of this paper is to highlight all of the key points that fall under the meaning of humanisation inside the ICU Liberation bundle.
Early Mobilisation
Patients admitted to the ICU can experience long periods of immobilisation which can lead to muscular decay. However, other factors may coexist and have a negative impact on muscular health, such as long sedation periods, inflammation, malnutrition, and use of neuromuscular blockade agents (NMBAs), among others. An important percentage of these patients will develop ICU-Acquired Weakness (ICUAW), an entity that can complicate functional prognosis (Saoirse et al. 2015; Hodgson et al. 2014; Zang et al. 2020; Vanhorebeek et al. 2020).
The diagnosis of ICUAW is commonly made through the Medical Research Council Sum-Score (MRC-SS <48 points), or by hand-grip strength measured with a dynamometre (<11 kg for males and <7 kg for females). Nowadays, there are other tools that can help identify patients with a high risk of developing ICUAW (Vanhorebeek et al. 2020). However, muscular ultrasound evaluation is one of the most promising methods. In ultrasound evaluation, quality and quantity can be measured over time. The Heckmatt scale will categorise, in a progressive manner, four different muscular situations. In addition, it would be of best practice to recognise the functional status previous to the ICU admission in order to establish a realistic prognosis.
One of the most important measures to prevent functional impairments is early mobilisation (EM). It stands for the application of physical activity in the first two to five days since the onset of critical illness, and active movement (made by the patient) is preferred over assisted or passive interventions (Saoirse et al. 2015; Hodgson et al. 2014). EM must be initiated based on a patient’s level of mobility (LOM) and strength. A common mistake made during EM is underestimating the patient’s capacity to perform or accomplish certain exercises and prescribing exercise as if patients had a lesser functional level. Therefore, the rehabilitation process can be ominous and with poor progression.
It is vastly known that EM is a safe practice in ICU patients. In well selected patients it can be applied even during mechanical ventilation (MV), extracorporeal membrane oxygenation (ECMO), continuous renal replacement therapy (CRRT), etc. (Hodgson et al. 2014). Patient safety should always be assured at all times, as well as a profound and continuous evaluation of patient stability. EM can generate positive changes in ICU practices and outcomes for the patient and their families, with analgesia optimisation, proper sedation levels, reduction in bedtime, delirium prevention and by reducing LOS inside the ICU and total MV and hospitalisation days (Zang et al. 2020).
Diverse functional scales have been validated for the critically ill patient. These allow the rehabilitation and ICU staff to understand the initial state of the patient, create an intervention strategy and continuously assess and restructure strategies over time. Regardless of the evaluation tool, functional evaluation must be protocolised as part of the physical examination in the critical patient. Measuring survival in the ICU is not enough for what today’s practice can offer; functionality needs to become one of the primary outcomes in order to talk about “quality of attention”. Human movement has to be the supreme therapeutic strategy for the rehabilitation staff and the physical therapist as an expert in this domain must be a key piece in the prevention and management of functional complications inside the ICU. Time does not forgive anything, not even the muscle.
Communication
Communication is one of the toughest aspects to establish in the ICU. Due to different medical equipment attached or introduced in the patient, isolation and the lack of importance given to communicating with the patient, in conjunction with the lack of expertise of the staff on this topic, hinders communication. Establishing solid communication lines with the patient and their family, along with good communication between the multidisciplinary team in charge of the patient’s care can simplify the understanding of the approach that will be set, and, likewise minimise the inhumane effects of the ICU (Rojas et al. 2014).
During invasive and non-invasive MV, devices are placed in the patient that can provoke the impossibility to use the structures that produce the voice, anatomical and/or functional alterations, even swallowing disorders. A solution for these cases is Alternative and Augmentative Communication (AAC). AAC consists, in conjunction, resources, systems or strategies that facilitate the comprehension and expression of language in people with speaking or writing impairments (Deliyore-Vega 2018). Its objective is to enlarge the speech or substitute it so that patients can express their thoughts, feelings, needs and wishes. It is fundamental that the ICU staff develops the capacity to utilise these alternatives of communication and their way around the chosen strategy to avoid frustration. In patients undergoing tracheostomy, the utilisation of devices that allow communication between upper and lower airway are recommended as an effort to permit oral communication (Fernández et al. 2012). All of these measures will enhance effective communication with family and the multidisciplinary team. An evaluation of communication needs is necessary to choose the adequate AAC.
The patient’s family is involved in the alterations suffered by critical illness and post-intensive care syndrome (PICS). Communication between the patient and their family is fundamental for the patient’s well-being and can be established through phone calls, video calls, writing or the utilisation of an AAC method. Integrating an open-door ICU programme can ease the communication process. Furthermore, families must have straightforward communication with the personnel in charge for the purpose of integrating them in the decision making process. Also, staff communication has to be dynamic at all times in order to establish the same objectives and approaches while considering the family and the patient’s point of view (Ayuso-Murillo et al. 2017).
Personal Care and Hygiene
Secondary to ICU admission, hygiene and self-care is lost in most cases and depends totally on healthcare staff and family members. Providing adequate hygiene and personal care routine, ensuring patient comfort and establishing proper hygiene habits can prompt humane practices for ICU patients. This can also make hospitalisation a more tolerant process and can improve the patient’s quality of life during this time. Respecting privacy, in some cases, is a lost habit as well. All of these practices and habits are easy to implement and can lessen some of the negative effects of the ICU (Carrascal et al. 2015; Cantón-Bulnes et al. 2019; Ross and Crumpler 2007; Estaji et al. 2015; Fields 2008). A list of hygiene and personal care measures is stated below:
• Facial and corporal hygiene (bathing, shaving, hair care, external genitalia hygiene, etc.).
• Tooth and dental prosthesis care and wash.
• Adequate bowel and urine collection and cleaning.
• Skin care; application of humectation creams and deodorant.
Recreation
Recreation in the critically ill is a forgotten aspect, but such a basic human need. “Let them concentrate on getting better” or “If the patient is having fun or laughing makes our work less professional and can seem to take away the seriousness” are some comments we can face while talking about this topic. Professional care together with making a comfortable and humane environment can be established in the same space. It’s no surprise that there is such a lack of information surrounding this subject and the need for more interest is evident. Some options have been studied like Virtual Reality (VR) as a recreation, anti-delirium and pain management strategy (González-Consuegra et al. 2016). Recreation must be a therapeutic measure to support an integral progress including physical, social, mental and emotional health. Moreover, recreation can become a linkage in adherence to occupational and physical therapy (Naef et al. 2021).
In any state, including the critically ill, recreation has to be variable and individualised due the heterogeneity in preferences and desires of patients. Creating a comfortable and enjoyable environment for people to recover from critical illness, or at least for some time during the day, can help the patient feel like themselves again and help them overcome what they are going through.
Examples of recreation strategies include:
• Cognitive stimulation: math work, logical thinking, memory games.
• Didactic activities: painting or craft making.
• Musical or visual stimulation: movies, VR or preferred music.
• Space and time orientation: calendar making that could include day to day happenings and important upcoming events.
Mental Wellbeing
Undergoing critical illness is a situation that forces individuals to face diverse duels in a cognitive and emotional matter (Costigan et al. 2019). Typically, in this topic delirium would be the centre piece of discussion. Delirium is a fundamental part of mental care and if established, it can trigger many alterations. However, delirium, in many cases, is the result of poor protection of a patient’s mental health (Wade et al. 2016). Adequate sedation practices, family empowerment, pain management and mobilisation are some worldwide known examples of how to overpower this condition (Slooter et al. 2017). Nonetheless, a hard pill to swallow is that delirium is not treated, it's prevented. If the personnel in charge of the ICU unite efforts in a multidisciplinary way, complications can be prevented, and so can delirium.
Many mental disorders like anxiety, depression and posttraumatic stress disorder are common while fighting critical illness and the need of personnel with expertise in this approach is undeniable (Trogrlić et al. 2015). It's worth noting that the instauration of any disorder will complicate health attention, restrain functionality, and overwhelm emotional status to the point patients can develop a death wish (Trogrlić et al. 2015; Kaneko-Wada et al. 2015). Alternatives such as thanatological follow-up and long-length family visits can modulate such disorders. Creating an open-door ICU would simplify these practices and could give the professionals involved in mental care a realistic perspective of what patients could face after ICU discharge.
Once the patient leaves the ICU, different cognitive problems have been observed over time. Memory loss, concentration difficulties, slow thinking and poor problem resolution are some of the most common. In fact, Pandharipande et al. (2013) found that one out of every four patients discharged underwent a similar cognitive impairment to Alzheimer’s in its moderate state. More so, worse global and executive cognitive outcomes were related with the length of delirium, despite sedation levels, analgesia, age and other conditions. Therefore, taking care of patients’ mental health is taking care of their future (Müller et al. 2020).
Analgesia and Sedation in Mechanically Ventilated Patients
Clinical practice guidelines for analgesia and sedation in the ICU (e.g., the Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption (PADIS) guidelines) have consistently focused on patient-oriented management of pain, minimum levels of sedation, early mobilisation (EM) and rapid liberation from MV. To achieve these goals, clinical assessment of pain and level of sedation with validated tools such as the Behavioral Pain Scale (BPS), the Critical-Care Pain Observational Tool (CPOT), and the Sedation Agitation Scale (SAS) or Richmond Agitation Sedation Scale (RASS), respectively should be conducted at least twice a day.
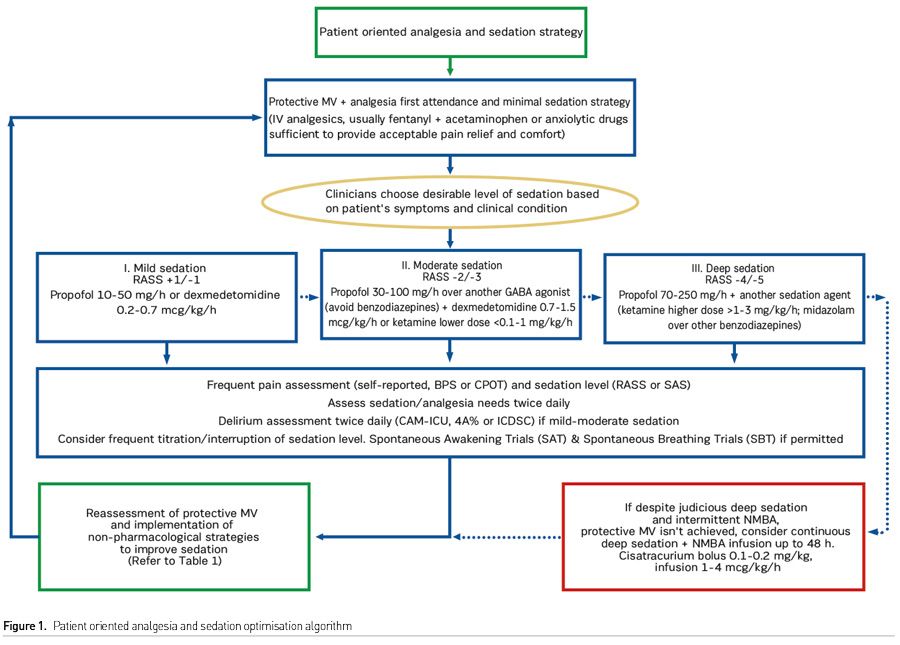
An adequate management of analgesia and sedation, based on patient centred attention; protective MV, analgesia first attendance and minimal sedation strategy (RASS +1/-1) must permit higher levels of activity that will reverberate positively in the incidence of ICUAW and delirium, sedative requirements, ICU LOS, pain intensity, duration of MV and weaning process from MV. To provide comfort, safety and acceptable pain relief are the primary goals from analgesia/sedation. Once they are in communion, the implementation of non-pharmacological strategies to facilitate EM and patient interaction with staff and family can be the path to earlier physical and cognitive recovery. Non-pharmacological recommendations that may result in benefit prior to the administration of new sedatives and NMBAs for MV patients are outlined in (Table 1.)

Even though the CPOT and the BPS remain the most robust scales for assessing pain in critically ill adults unable to self-report, other technologies that may be useful in the ICU pain and sedation assessment process should be explored. Technology measuring heart rate variability (e.g., the Analgesia Nociception Index), electroencephalographic signals (e.g., the Bispectral Index), and pupillary reflex dilation using video pupillometry have shown promising results in analgesia/sedation assessment of critically ill adults, but future research is necessary to determine the benefits, harms, and feasibility of implementation in the ICU.
It is also worth mentioning that in a great number of patients, deeper levels of sedation in the first 48 hours after admission to the ICU remains frequent due to life threatening conditions (Slooter et al. 2017), like severe acute respiratory distress syndrome (ARDS), non-resolved status epilepticus (SE), intraabdominal hypertension (IAH), flail chest (FC), etc. In these cases, deep sedation level (RASS -4/-5) should be systematically achieved, as recommended in Figure 1, to secure lifesaving interventions without putting aside the assessment and management of analgesia/sedation, non-pharmacological strategies to prevent delirium and the primal core of patient-oriented sedation and analgesia strategy, analgesia first attendance and minimal sedation (RASS +1/-1) as soon as the clinical condition of the patient allows it.
Non-Pharmacologic Interventions to Prevent Delirium
Delirium is a common acute brain dysfunction that affects critically ill patients. Even though delirium was first described 50 years ago, it still remains an underdiagnosed condition in the ICU. In a recent systematic review published by Wilson et al. (2020), delirium was defined as “a syndrome characterised by an acute change in attention, awareness and cognition, caused by a medical condition that cannot be better explained by a pre-existing neurocognitive disorder.” Multiple predisposing factors and several neurobiological processes that contribute to delirium pathogenesis are well exposed.
Evidence has been described in order to prevent, manage or treat delirium in important programmes such as the PADIS guidelines and the ICU Liberation (ABCDEF) bundle. In both of these, EM plays an important role to overpower many of the consequences of critical illness, such as delirium. Delirium prevention and management needs a multidisciplinary approach with routine delirium assessment and standardised EM protocols that are intimately related with minimising sedation, which means both spontaneous awakening trial (SAT) and spontaneous breathing trial (SBT) need to be in coordination (Trogrlićet al. 2015).
Delirium has been associated with an increase in morbidity, mortality, LOS in the ICU and long-term cognitive impairment (Herling et al. 2018). Therefore, the need to assess and identify it is evident. The most common and preferred method to diagnose delirium in the ICU is the CAM-ICU. Delirium rates vary depending on the population that is studied and over the interaction of other 100 risk factors described in the literature.
The implementation of the correct measures for the prevention of delirium must be perceived with an equally reverberating power such as decrease in sedation (specially with the use of benzodiazepines), analgesic optimisation in the presence of pain (supporting non-pharmacological measures), considering physiological sleeping time (avoiding nocturnal procedures), allowing sunlight exposure, avoiding restraints or any movement restriction and establishing effective communication channels between patient-staff and patient-family (Pandharipande et al. 2010; Devlin et al. 2018; Inoue et al. 2019; Smonig et al. 2019). A list of non-pharmacological strategies to prevent and manage delirium is described in (Table 2).

Family Commitment and Empowerment
Frequently, it is perceived that the presence of family interferes with the work of healthcare providers (Smonig et al. 2019; Phipps et al. 2007; Weaver et al. 2012). Nonetheless, some benefits have been reported such as decrease in agitation, anxiety, confusion, clinical complications, LOS and a long-term improvement in cognitive performance. Additionally, there is a reduction in financial costs due to minimised time inside ICU and hospital, and reduction in clinical cognitive comorbidities (Heyland et al. 2016; Toneli et al. 2010). Moreover, other studies have found that the presence of a family member during CPR is associated with positive psychological effects like anxiety discount in those already mentioned. Along with this, understanding the effort being made by the personnel to preserve the patient’s life helped reduce LOS and legal conflicts were minor compared to non-present CPR (Fumagalli et al. 2006; Pun et al. 2021; Maclean et al. 2003; Compton et al. 2005; Halm et al. 2005; Terzi et al. 2008).
Methodically to have a satisfactory active participation of the family inside the ICU, instruction, education and cultural changes are needed. Also, family roles and functions, procedure explanation and possible outcomes should be explained to have an adequate dynamic. Social workers, nurses or other health care providers can serve as a bridge between ICU attendance and family if they have full understanding of the situation (Weaver et al. 2012).
Within the family roles, “decision making” is a corner stone. Basically, it's taking the decision over receiving or not receiving certain interventions. A vast and easy understanding by the patient is needed to accomplish this properly (Weaver et al. 2012; Heyland et al. 2018). Shared family decision has to be an option to endure the stress of facing critical illness (Meyers et al. 2000; Trees et al. 2017; Buckey et al. 2012).
Accomplishing this role is tough when the patient is close to the end of their life, and an adequate coordination between the family is primordial. End of life decisions include initiating, continuing, containing or ending vital life support. The lack of family involvement in decision making is associated with unnecessary medical procedures and conflicts with the care taking staff (Meyers et al. 2000; Trees et al. 2017; Buckey et al. 2012). The key to this is exceptional communication.
A fundamental part of family empowerment is reducing the risk of PICS as much as possible. PICS will affect the family if the patient cannot overcome critical illness. Without a doubt, the patient's family has a huge role to play and should be part of the multidisciplinary team. They are the ones who really appreciate the previous and actual state of the patient, their values, preferences and wishes. Together, decision-making and PICS prevention can improve patient outcomes and assure treatment adherence (Weaver et al. 2012; Heyland et al. 2018: Halm et al. 2005; Azoulay et al. 2003; Rodriguez et al. 2008). Henceforth, there is no place with a major need of active family participation than the ICU.
Conclusion
Providing humane practices will benefit everybody involved in the attention of a critically ill patient. The application of such practices can be easy to implement and with a low cost. The perception of the patient as a biological, psychological and social being is crucial for this matter. Opening the ICU for family members as well as accepting help from the whole multidisciplinary personnel is the only way of assuring a complete and integral approach. Humanised healthcare is a patient right, a family need and a healthcare obligation. H-ICU is the only way of structuring a high-grade ICU.
Conflict of interest
None. 

References:
Ayuso-Murillo D, Colomer-Sánchez A, Herrera-Peco I (2017) Communication skills in ICU and adult hospitalisation unit nursing staff. Enferm Intensiva, 28(3):105-113. doi: 10.1016/j.enfi.2016.10.006.
Azoulay E, Pochard F (2003) Communication with family members of patients dying in the intensive care unit. Curr Opin Crit Care, 9(6):545-50. doi: 10.1097/00075198-200312000-00014.
Buckey JW, Molina O (2012) Honoring patient care preferences: surrogates speak. Omega (Westport), 65(4):257-80. doi: 10.2190/OM.65.4.b.
Carrascal GC, Ramírez M, Juan D et al. (2015) Hygiene: basic care that promotes comfort in critically ill patients. Revista electronica trimestral de enfermería, 14(4):1695-6141.
Cantón-Bulnes ML, Garnacho-Montero J (2019) Oropharyngeal antisepsis in the critical patient and in the patient subjected to mechanical ventilation. Med Intensiva, 43 Suppl 1:23-30. doi: 10.1016/j.medin.2018.06.011
Compton S, Madgy A, Goldstein M et al. (2006) Emergency medical service providers' experience with family presence during cardiopulmonary resuscitation. Resuscitation, 70(2):223-8. doi: 10.1016/j.resuscitation.2005.12.012.
Costigan FA, Duffett M, Harris JE et al. (2019) Occupational therapy in the ICU: A scoping review of 221 documents. Crit Care Med., 7(12):e1014–21
Deliyore-Vega M (2018) Alternative Communication: A Tool for Social Inclusion of People with Disabilities. Revista Electrónica Educare, 22(1), 1-16. doi.org/10.15359/ree.22-1.13
Devlin JW, Skrobik Y, Gélinas C et al. (2018) Clinical Practice Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the ICU. Crit Care Med., 46(9):e825-e873. doi: 10.1097/CCM.0000000000003299.
Estaji Z, Alinejad M, Rakhshani HM (2015) The Comparison of Chlorhexidine Solution and Swab With Toothbrush and Toothpaste Effect on Preventing Oral Lesions in Hospitalized Patients in Intensive Care Unit. Glob J Health Sci.,8(5):211-6. doi: 10.5539/gjhs.v8n5p211.
Fernández A, Peñas L, Yuste E, Díaz A (2012) Exploración y abordaje de disfagia secundaria a vía aérea artificial. Med Intensiva, 36(6):423-33.
Fields LB (2008) Oral care intervention to reduce incidence of ventilator-associated pneumonia in the neurologic intensive care unit. J Neurosci Nurs.,40(5):291-8. doi: 10.1097/01376517-200810000-00007.
Fumagalli S, Boncinelli L, Lo Nostro A et al. (2006) Reduced cardiocirculatory complications with unrestrictive visiting policy in an intensive care unit: results from a pilot, randomized trial. Circulation. 21;113(7):946-52. doi: 10.1161/CIRCULATIONAHA.105.572537
González-Consuegra RV, Pérez Valderrama DC, Valbuena-Flor LF (2016) Prevención de lesiones de piel: educación en el equipo de salud y familiares de personas hospitalizadas. Rev. Fac. Med., 64(2):229-38
Grupo de trabajo de certificación de proyecto HU-CI (2017) Manual de buenas prácticas de humanización en unidades de cuidados intensivos. Madrid proyecto HU-CI. Available from
humanizandoloscuidadosintensivos.com/es/buenas-practicas/
Halm MA (2005) Family presence during resuscitation: a critical review of the literature. Am J Crit Care, 14(6):494-511.
Herling SF, Greve IE, Vasilevskis EE et al. (2018) Interventions for preventing intensive care unit delirium in adults. Cochrane Database Syst Rev., 11(11):CD009783. doi: 10.1002/14651858.CD009783.pub2.
Heyland DK, Davidson J, Skrobik Y et al. (2018) Improving partnerships with family members of ICU patients: study protocol for a randomized controlled trial. Trials. 19(1):3. doi: 10.1186/s13063-017-2379-4.
Hodgson CL, Stiller K, Needham DM et al. (2014) Expert consensus and recommendations on safety criteria for active mobilization of mechanically ventilated critically ill adults, Critical Care. doi: 0.1186/s13054-014-0658-y
Inoue S, Hatakeyama J, Kondo Y et al. (2019) Post-intensive care syndrome: its pathophysiology, prevention, and future directions. Acute Med Surg., 6(3):233-246. doi: 10.1002/ams2.415. PMID: 31304024
Kaneko-Wada F de JT, Domínguez-Cherit G et al. (2015) The process of death in the intensive care unit (ICU). From a medical, thanatological and legislative point of view. Gac Med Mex., 151(5):628–34.
Maclean SL, Guzzetta CE, White C et al. (2003) Fontaine D, Eichhorn DJ, Meyers TA, Désy P. Family presence during cardiopulmonary resuscitation and invasive procedures: practices of critical care and emergency nurses. J Emerg Nurs.,29(3):208-21. doi: 10.1067/men.2003.100.
Meyers TA, Eichhorn DJ, Guzzetta CE (2000) Family presence during invasive procedures and resuscitation. Am J Nurs., 100(2):32-42; quiz 43.
Müller A, von Hofen-Hohloch J, Mende M et al. (2020) Saur D, Fricke C, Bercker S, et al. Long-term cognitive impairment after ICU treatment: a prospective longitudinal cohort study (Cog-I-CU). Sci Rep., 10(1):15518
Naef AC, Jeitziner M-M, Gerber SM et al. (2021) Virtual reality stimulation to reduce the incidence of delirium in critically ill patients: study protocol for a randomized clinical trial. Trials, 22(1):174
Pandharipande PP, Girard TD, Jackson JC et al. (2013) Long-term cognitive impairment after critical illness. N Engl J Med., 369(14):1306–16
Pandharipande P, Banerjee A, McGrane S et al. (2010) Liberation and animation for ventilated ICU patients: the ABCDE bundle for the back-end of critical care. Crit Care., 14(3):157. doi: 10.1186/cc8999.
Phipps LM, Bartke CN, Spear DA et al. (2007) Assessment of parental presence during bedside pediatric intensive care unit rounds: effect on duration, teaching, and privacy. Pediatr Crit Care Med., 8(3):220-4. doi: 10.1097/01.PCC.0000262798.84416.C
Pun BT, Badenes R, Heras La Calle G et al. (2021) Prevalence and risk factors for delirium in critically ill patients with COVID-19 (COVID-D): a multicentre cohort study. Lancet Respir Med.,9(3):239-250. doi: 10.1016/S2213-2600(20)30552-X.
Radwany S, Albanese T, Clough L (2009) Sims L, Mason H, Jahangiri S. End-of-life decision making and emotional burden: placing family meetings in context. Am J Hosp Palliat Care,(5):376-83. doi: 10.1177/1049909109338515.
Rodriguez RM, Navarrete E, Schwaber J (2008) A prospective study of primary surrogate decision makers' knowledge of intensive care. Crit Care Med., 36(5):1633-6. doi: 10.1097/CCM.0b013e31816a0784.
Rojas NP, Bustamante-Troncoso CR, Dois-Castellón A (2014) Comunicación entre equipo de enfermería y pacientes con ventilación mecánica invasiva en una unidad de paciente crítico. Aquichan, 14(2): 184-195.
Ross A, Crumpler J (2007) The impact of an evidence-based practice education program on the role of oral care in the prevention of ventilator-associated pneumonia. Intensive and Critical Care Nursing, 23:132-136
Saoirse C, Ball I, Cepinskas G et al. (2015) Early Mobilization in the Critical Care Unit: A Review of Adult and Paediatric Literature, Journal of Critical Care. doi:10.1016/j.jcrc.2015.03.032
Shehabi Y, Bellomo R, Kadiman S et al. (2018) Sedation Intensity in the First 48 Hours of Mechanical Ventilation and 180-Day Mortality: A Multinational Prospective Longitudinal Cohort Study. Crit Care Med., 46(6):850-859. doi: 10.1097/CCM.0000000000003071.
Slooter AJC, Van De Leur RR et al. (2017) Delirium in critically ill patients. Handb Clin Neurol., 141:449–66
Smonig R, Magalhaes E, Bouadma L et al. (2019) Impact of natural light exposure on delirium burden in adult patients receiving invasive mechanical ventilation in the ICU: a prospective study. Ann Intensive Care. 9(1):120. doi: 10.1186/s13613-019-0592-x.
Terzi AB, Aggelidou D (2008) Witnessed resuscitation: beneficial or detrimental? J Cardiovasc Nurs., 23:74–8.
Tonelli MR, Misak CJ (2010) Compromised autonomy and the seriously ill patient. Chest. 137(4):926-31. doi: 10.1378/chest.09-1574.
Trees AR, Ohs JE, Murray MC (2017) Family Communication about End-of-Life Decisions and the Enactment of the Decision-Maker Role. Behav Sci (Basel), 7(2):36. doi: 10.3390/bs7020036.
Trogrlić Z, van der Jagt M et al. (2015) A systematic review of implementation strategies for assessment, prevention, and management of ICU delirium and their effect on clinical outcomes. Crit Care.,19(1):157
Vanhorebeek I et al. (2020) ICU-acquired weakness. Intensive care medicine, 46(4): 637-653. doi:10.1007/s00134-020-05944-4
Wade DF, Moon Z, Windgassen SS et al. (2016) Non-pharmacological interventions to reduce ICU-related psychological distress: a systematic review. Minerva Anestesiol., 82(4):465–78
Weaver JL, Bradley CT, Brasel KJ (2012) Family engagement regarding the critically ill patient. Surg Clin North Am., 92(6):1637-47. doi: 10.1016/j.suc.2012.08.004.
Wilson JE, Mart MF, Cunningham C et al. (2020) Delirium. Nat Rev Dis Primers. 6(1):90. doi: 10.1038/s41572-020-00223-4. Erratum in: Nat Rev Dis Primers.
Zang K, Chen B, Wang M et al. (2020) The effect of early mobilization in critically ill patients: A meta-analysis. Nurs Crit Care, (6):360-367. doi: 10.1111/nicc.12455.

























