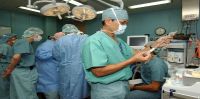
"The operating room is a very fast-paced, high-demand, all senses
running on all cylinders type of environment," said study coauthor
Matthew Bush, MD, assistant professor of surgery at the University of
Kentucky Medical Center, Lexington. "To minimize errors of
communication, it is essential that we consider very carefully the
listening environment we are promoting in the OR."
To assess the effects of ambient noise on communication in the OR,
the researchers created a noise environment similar to that of an OR and
tested 15 surgeons with one to 30 years of operating experience. The
surgeons' ability to understand and repeat words was tested using the
Speech In Noise Test-Revised (SPIN-R) under four different listening
conditions typical of OR environments. These conditions included quiet,
filtered noise through a surgical mask and background noise both with
and without music. Subjects were tested in two situations: engaged in a
specific surgical task and task free.
The study showed a significant decrease in speech comprehension with
the presence of background noise when the words were unpredictable. In
addition, the surgeons demonstrated considerably poorer speech
comprehension in the presence of music compared with a quiet environment
or one with OR noise present. However, the addition of music became a
significant barrier to speech comprehension only when the surgeon was
engaged in a task.
The researchers concluded that OR noise can cause a decrease in
auditory processing, particularly in the presence of music. Further,
the ability to understand what is being said becomes even more difficult
when the conversations carry critical information that is
unpredictable.
Currently, miscommunication is one of the most frequently cited
causes of preventable medical errors. For this reason, there is a
growing interest in identifying overlooked variables that can lead to
communication breakdowns among health care professionals.
Therefore, these study results have important implications in the
real world because surgical teams carry on critical conversations during
surgical procedures that often include discussions about medications
and dosing as well as the blood supply that should be on hand. Because
some of these details might sound similar, clear communication is
crucial to avoiding medical errors (i.e.: a request for the drug heparin
might be heard as Hespan).
"Our main goal is to increase awareness that operating room noise
does affect communication and that we should foster the best environment
in which we can communicate better," Dr. Bush explained. "This effort
means that the surgical team needs to work diligently to create the
safest environment possible, and that step may mean either turning the
music off or down, or limiting background conversations or other things
in the environment that could lead to communication errors and medical
mistakes."
In future studies, the researchers plan to look at a larger population of surgeons, especially those who are hearing impaired, as well as other operating team members such as anesthesiologists and nurses.
"I think it's important to demonstrate the effect of environmental operating noise on communication on a variety of different players in the operating room setting," Dr. Bush said. "Another step from here is to not only see how noise affects our understanding of speech, but how it affects our tasks, how it affects our ability to perform surgical procedures efficiently and effectively. That is a different stage and different study design completely, but these questions are all ahead of us as we investigate the effects of environmental sound on operating room communication."
Other study investigators include T. Justin Way, MD; Ashleigh Long,
PhD; Jeff Weighing, PhD, Rosalind Ritchie, MD; Raleigh Jones, Jr., MD;
Jennifer B. Shinn, PhD.
Source: EurekAlert!