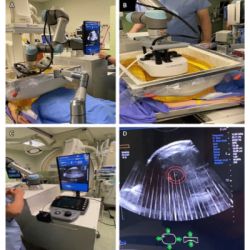
A recent pilot study highlighted the promising results of a novel imaging system using two-photon-fluorescence microscopy (TPFM). The results are highlighted in a pilot study, summarised in JAMA Dermatology.
During regular skin lesion biopsies for non melanoma skin cancer, a physician will examine the pathology under a microscope and depending on what can be seen, the patient may have to return for a second appointment. However, this novel imaging system allows a surgeon to immediately decide whether the lesion is cancerous so that patients can be treated during the same visit. Hence, the process is remarkably shortened.
During the pilot study, the system was tested on 15 biopsies of known non melanoma skin cancer. It detected basal carcinoma with full accuracy and detected squamous cell carcinoma with very high accuracy.
Typically the process to evaluating biopsied tissue is very slow. Waiting for biopsy results is very time consuming for the patient and the surgeon, taking up time spent in the operating room.
However, this system has the potential to quickly provide biopsy results for all kinds of diseases.
Michael Giacomelli, assistant professor of biomedical engineering and of optics at the University of Rochester, provided a good example of how this technology works.
He says, “You see random cases where they take out the prostate, and sometimes there's an obvious tumor that has spread beyond the prostate, or other times it is very localized. This technology offers a possibility to adjust the patient's therapy on the fly”.
TPFM not only generates high-resolution images, but it can also penetrate deep through tissue using near-infrared light. This makes it advantageous for fast imaging of biopsies without much needed preparation.
In addition,Giacomelli is running a parallel study to investigate whether a system incorporating TPFM and video can both be used to guide surgeries.
The system overlays TPFM images of the point where the tissue is being removed on a webcam image.
As Giacomelli explains, “You can show what the excised tissue looks like, and how much of the tumor is located on the excision”.
“They can then map that back into the wound that they are creating in order to decide which side to cut”.
Source: University of Rochester
Image Credit: iStock
References:
Vincent D et al. (2022) Real-time Analysis of Skin Biopsy Specimens With 2-Photon Fluorescence Microscopy. JAMA Dermatology.