An extensive group of researchers from Germany, led by Dr Monika Graeser, from the Department of Gynecology, University Hospital Leipzig, presented results on “Magnetic resonance imaging and ultrasound for prediction of residual tumor size in early breast cancer within the ADAPT subtrials.” The West German Study Group (WSG) conducted this imaging project in the framework of the Adjuvant Dynamic Marker-Adjusted Personalized Therapy Trial Optimizing Risk Assessment and Therapy Response Prediction in Early Breast Cancer (ADAPT) umbrella trial.
The aim of this study was to identify early markers for therapy response to individualise post-neoadjuvant therapy (NAT) by avoiding over- and under-treatment. Predicting histological tumour size by post-neoadjuvant therapy (NAT) ultrasound and magnetic resonance imaging (MRI) was evaluated in different breast cancer subtypes.
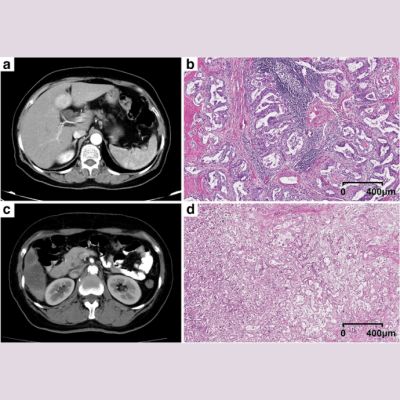
After 12 weeks of post-neoadjuvant therapy, imaging was carried out on patients enrolled in three neo-adjuvant ADAPT sub-trials. The images were analysed to predict residual tumour measuring ≤10 mm and summarised using positive (PPV) and negative (NPV) predictive values. The results of the 248 patients who had MRI and 588 who had ultrasound provided insightful data. Tumour size was over- or underestimated by < 10 mm in 4.4% and 21.8% of patients receiving MRI; and 10.2% and 15.8% for ultrasound.
The negative predictive values (share of correctly predicted tumour size ≤10 mm) of MRI and ultrasound was 0.92 and 0.83. PPV (correctly predicted tumour size > 10 mm) was 0.52 and 0.61. MRI showed a higher NPV and lower PPV than ultrasound in hormone receptor (HR)-positive/human epidermal growth factor receptor 2 (HER2)-positive and in HR−/HER2+ tumours. In HR−/HER2− tumours, the NVP and PPV for both methods were comparable.
This study showed that MRI is less likely than ultrasound to underestimate tumour size for HR+/HER2+ and HR−/HER2+ breast cancer. Ultrasound shows a lower risk to overestimate tumour size. Both ultrasound and MRI are accurate in predicting residual tumour material after NAT in HR+/HER2+ and HR−/HER2−BC.
However, in HR+/HER2+ and HR−/HER2+ breast cancer, MRI is less likely than ultrasound to underestimate while ultrasound is associated with a lower risk to overestimate tumour size. These findings may help to select the most optimal imaging approach for planning surgery after NAT. these findings could help to select the optimal imaging modality, interpreting result and planning surgery for patients with incomplete imaging response to NAT.
Source: NCBI
Image credit: iStock