ICU Management & Practice, Volume 21 - Issue 2, 2021
Nowadays, we are facing some important facts: there has been a global increase of sepsis worldwide over the last decades (Rudd et al. 2020; Angus et al. 2001), sepsis-related mortality and morbidity are major healthcare problems (Fleischmann et al. 2016; Duganiet al. 2017) and the proportion of very old patients with sepsis is increasing substantially in our hospitals due to ageing of the population (Martin et al. 2006; Ferrer et al. 2008; Flatten et al. 2017; Fernando et al. 2019). The incidence of sepsis increases with age, up to 67% of septic patients are aged > 65 years, with a particular relevance in subjects ≥80 years (Lee et al. 2018). Consequently, sepsis represents 10-14% of intensive care units (ICUs) acute admissions in very old people (Ibarz et al. 2020).
Nevertheless, despite the increased trend in incidence, observational studies have reported a decrease in mortality associated with severe sepsis (Fleischmann et al. 2016). In Spain, a large retrospective analysis of a 5-year period (2008–2012) in patients hospitalised with sepsis reported a yearly increase incidence of 7% while a relative annual reduction in length of stay and in-hospital mortality of 3.3% and 3.4% respectively (Yebenes et al. 2017). In a nationwide study in Taiwan, sepsis admissions increased from 4% (2002) to 9% (2012) while in-hospital mortality rate decreased from 24% to 14.8%; and this decrease was similar in adult, elderly and oldest old groups (Lee et al. 2018). In an Italian general hospital, case fatality rate in sepsis decreased particularly in subjects ≥80 years (Fabri et al. 2019). A quick and aggressive resuscitation plan has proven to reduce mortality in sepsis patients, not only in young ones but also in those that are usually considered for a less-intense treatment which includes our very old patients.
Sepsis is defined as life-threatening organ dysfunction caused by a dysregulated host response to infection (Singer et al. 2016). It can be lethal, but it is a continuum of disease severity and it is treatable. An early identification and timely implementation of targeted interventions improves outcomes (Seymour et al. 2017). The World Health Assembly has urged member states to strengthen efforts to identify, document, prevent and treat sepsis (Reinhart et al. 2017).
Sepsis in the Oldest Old
I am called to the emergency room to assess a patient with sepsis. The patient is an 82-year-old man with a presumed urinary tract infection. He was discharged from hospital one month ago with a permanent urinary catheter for haematuria. He lives with his wife, his cognition is adequate for his age, he goes out with his wife to do some shopping and takes care of the usual monetary affairs. He has some comorbidities (hypertension, cardiac insufficiency, arthritis, hypoacusis) but all of them are well controlled. He takes four medications. On physical exam, he is stuporous, hypertensive and tachypnoeic. His analysis shows elevated acute phase reactants, mild kidney failure and mild hypoxaemia. Has he got a sepsis? Should I admit him to the ICU? Would it be useful? What are his and his wife’s preferences? Which items should I consider?
The risk of dying from sepsis increases considerably with age; hospital mortality for patients >80 years of age is almost twice that of patients ≤ 50 years of age (Kotfis et al. 2019). A systematic review, including 18 studies and 4256 patients aged ≥ 80 years admitted to the ICU with sepsis reported mortality rates of 43% in the ICU, 47% in the hospital, and 68% 1 year after ICU admission (Haas et al. 2017). In a recent prospective, observational, multicentre study (Ibarz et al. 2020), ICU and 30-day mortality were 28.4% and 42%, respectively.
Early identification and treatment of sepsis are the major challenges in treating sepsis in our very old patients. First, they are at particularly high risk of developing sepsis due to pre-existing comorbidities, impaired immune function (immunosenescence), sarcopenia, decrease in reserve capacities related to ageing, and very often malnutrition and polypharmacy. Second, the oldest old often present nonspecific signs of infection, and clinical diagnosis of sepsis is usually more difficult. Confusion or falls can be the only sign; heart failure and arrhythmias are frequent, and differentiating infection from congestive heart failure can be difficult. On the contrary, few of the signs usually associated with sepsis are present; fever is absent in approximately 40% of older adults with infection. Third, emergency physicians are unlikely to refer octogenarian patients to the ICU and intensivists are reluctant to admit them due to the high morbidity and mortality and limited resources. Last but not least, we cannot forget to ask about the preferences of patients/relatives and be honest about our patient’s possibilities of recovering when establishing a plan of treatment.
The overall management of sepsis is similar for everyone (Rhodes et al. 2017; Levy et al. 2018), regardless of the age of the patient. It focuses on prompt recognition, early treatment with broad-spectrum antibiotics, control of infectious sources and resuscitation with intravenous fluids and vasopressors for patients with low blood pressure or elevated lactate. However, we should consider a few specific items in the oldest old. They have a lower cardiac compliance, and the renal perfusion is more cardiac flow dependent; thus, the management of fluid therapy is more sensitive (instead of 30ml/kg we should try 250 ml or repeated 100ml bolus). Their brain and kidney are especially vulnerable to insults and, consequently, careful sedation and prevention of delirium and acute kidney injury are mandatory. It is especially important to adopt non-pharmacological measures to prevent delirium from the very first moment they are admitted in the ICU and reduce the days of mechanical ventilation and sedation to a minimum. We cannot forget to ask if they wear glasses or hearing aids as sensory deficits create a predisposition to delirium. It is very important to maintain the circadian rhythm with daytime stimulation, time-space orientation, and a good night's sleep. Early mobilisation and respiratory physiotherapy will help to prevent or minimise muscle atrophy. Regarding antibiotics, we should consider pharmacodynamics and pharmacokinetics as oldest old have decreased systemic perfusion and are more sensitive to liver and kidney toxicities. In addition, dosing should sometimes be adjusted as their gastric emptying is slowed, glomerular filtration rate is decreased, and they have a reduced lean body mass, increase body fat, and a decrease in serum albumin which could cause increases in serum levels of drugs.
Risk Factors and Frailty
Some risk factors for mortality and morbidity in old patients with sepsis have already been identified and published: frailty, pre-existing co-morbidities, pre-hospitalisation dependency, presence, and severity of acute organ failure (SOFA), non-surgical status and prompt adherence of the bundles, in particular to the resuscitation bundle.
Frailty is present in approximately 40% of old people admitted to intensive care units and it is independently related to mortality and morbidity (Fernando et al. 2019; Flatten 2017; Guidet 2020). The term clinical frailty applies to a state or syndrome of reduced physical, physiologic, and cognitive reserve (Clegg et al. 2013). It is not an exclusive condition of old-aged people, but its prevalence increases with age being 25% of those over 65 years and over 50% in patients > 80 years. Frail patients are characterised by weakness, diminished motility, reduced muscle mass, decreased cognitive function and poor nutritional status in different intensity. Their capacity to respond to disease is diminished due to a failure of compensatory mechanisms to extrinsic stressors. If we consider frailty as a syndrome, it will be composed of several items: sarcopenia, changes in endocrine system, altered cognition, and immunosenescence.
Sarcopenia is defined as the age-associated loss of skeletal muscle mass which means less protein reserves. It could be more or less evident in daily life but definitely increases post-ICU neuro/myopathy and the days to wean from ventilator. As a consequence, this contributes to a longer ICU and hospital length of stay with increased morbidity and mortality. Many factors are associated with sarcopenia. Changes in endocrine system associated with ageing as higher concentrations of cortisol, a decreased level of testosterone and a decrease of growth hormone affect the normal function of muscle, tissue, and bone.
Regarding cognition, there is a loss of neurons with age mainly in hippocampus, which is related to cognitive decline and dementia. A common complication of critical illness is an increase in psychological symptoms, sleep cycle alterations, delirium, and cognitive impairment. Delirium is an independent risk factor associated with mortality.
And, what about immunosenescence? Ageing is also associated with a gradual deterioration of the immune system and a higher level of proinflammatory cytokines secretion at baseline. The pathophysiology of this immunosenescence is complex and multifactorial (Lang et al. 2010). Due to a chronic hyperstimulation of the immune system components all immunocompetent cells are affected, mainly adaptive cell-mediated immunity. The thymus atrophies with age, loses most of its activity within 60 years causing a shift in the T-cells, from naïve T-cells to memory T-cells. In response to antigens, these memory cells have limited proliferative capacity, express fewer co-stimulatory molecules, and lead to reduced activation of mitogen-activated protein kinase 2. Polyspecific, low affinity T-cell independent immunoglobulin levels increase with age and some of these immunoglobulins behave as autoantibodies. There is also a decreased ability to produce specific opsonophagocytic antibodies against neoantigens. Concerning innate immunity, macrophages undergo significant functional alteration, there is reduced antigen processing and expression to T cells, a reduced bactericidal activity and the expression and function of toll-like receptors is altered. Neutrophils and natural killer cells are also impaired causing reduced recognition and destruction of infected cells.
Frailty has lastly been proposed as a good candidate tool for ICU triage and should be added to risk stratification of old patients (Fernando et al. 2019; Flatten et al. 2017). Severity scores were not designed for old people and do not consider this issue. A simple and quick score, Clinical Frailty Scale (CFS) (Rockwood et al. 2005) can assess the present frailty level before hospital admission, not affected by the acute illness, and can be a huge help in identifying those patients more likely to survive sepsis. The information is easy to collect and the interrater reproducibility is very good, confirming that this tool is robust and easy to use (Guidet et al. 2020). The information necessary to perform this assessment can be given by patients or relatives or even taken from hospital records. The scale is composed of 9 classes from very fit to terminally ill. Prefrail patients have a CFS of 4, while frail patients have a CFS of 5 or above (Figure 1).

Sepsis Related Factors
The most frequent infections are lower respiratory and urinary tract infections (Lee et al. 2018; Yebenes et al. 2019); urinary sepsis has the lowest risk of death. Alternatively, other authors remark the intrabdominal origin (Martin-Loeches et al. 2019) which frequently implies an urgent diagnosis and a surgical intervention with high mortality. Bacteraemia is present in 30-40% of the cases.
The most common pathogens are gram negative and less frequently gram-positive. The most frequently isolated microorganism in cases of urinary sepsis is E. coli; but Proteus spp., Klebsiella spp. and Pseudomonas spp. are more prevalent in patients over 65 years old. We must also consider the possibility of an infection from multidrug-resistant organism, especially in the presence of previous hospitalisation, long-term care facilities, comorbid conditions (COPD, renal failure, diabetes mellitus), previous antibiotics or permanent devices. Besides this, there is a trend in the last decade of high incidence of fungal infections which the authors suggest is associated to age-related physiological changes, immune status, use of indwelling catheters, prolonged use of antibiotics, use of corticosteroids and chemotherapy (Lee et al. 2018).
Regarding organ dysfunction associated with sepsis, in addition to cardiovascular dysfunction, acute respiratory failure and renal dysfunction have been reported as the most prevalent (Yebenes et al. 2019; Lee et al. 2018). Maybe, there is an interaction between pre-existing comorbidity and acute organ dysfunction. That is to say, a patient with a chronic renal failure is more likely to develop acute renal failure during sepsis and similarly a patient with a chronic pulmonary disease is more prone to develop respiratory failure or difficult weaning from the ventilator. Undoubtedly, septic shock and more than two organs failing considerably increases mortality.
Life Sustaining Treatment Limitations
Life sustaining treatment (LST) limitations, regarding withholding or withdrawing, are more frequent in very old people. In VIP 1 study (Flatten et al. 2017), LST limitation was identified in 27% of patients and was associated with age, frailty and severity of illness (SOFA score). Considering only acute admissions, LST limitations were present in 32% and in 37% of patients admitted for sepsis, both similar in VIP2 study results (Guidet et al. 2020).
Such decisions should be individualised, and some considerations are important. First, LST is not equivalent to end of life decision. Second, the timing to take the decision is arbitrary, it can be before admission or at any time during hospitalisation. An ICU trial should be offered to very old patients, according to their previous health, frailty, comorbidities, and patient/relatives’ preferences. Third, the decision should probably include not only survival possibilities but also post-discharge functional capacity and quality of life. Fourth, the opinion of family members (or caregivers) is important, and we should hold a daily and sincere conversation about clinical condition and evolution (Kerckhoffs et al. 2020).
Is Sepsis an Independent Risk Factor for Mortality in Very Old Patients?
We studied the very old (≥80 years) septic patients in a large prospective multinational European study in 307 ICUs in 21 European countries (Ibarz et al. 2020). It was a sub-study of the VIP1 study. The VIP (very old intensive care patients, ≥80 years) network has conducted and published two large prospective observational studies (Flatten et al. 2017; Guidet et al. 2020), and several sub-studies; and in 2017 published a very old research agenda in which sepsis was one of the main subjects.
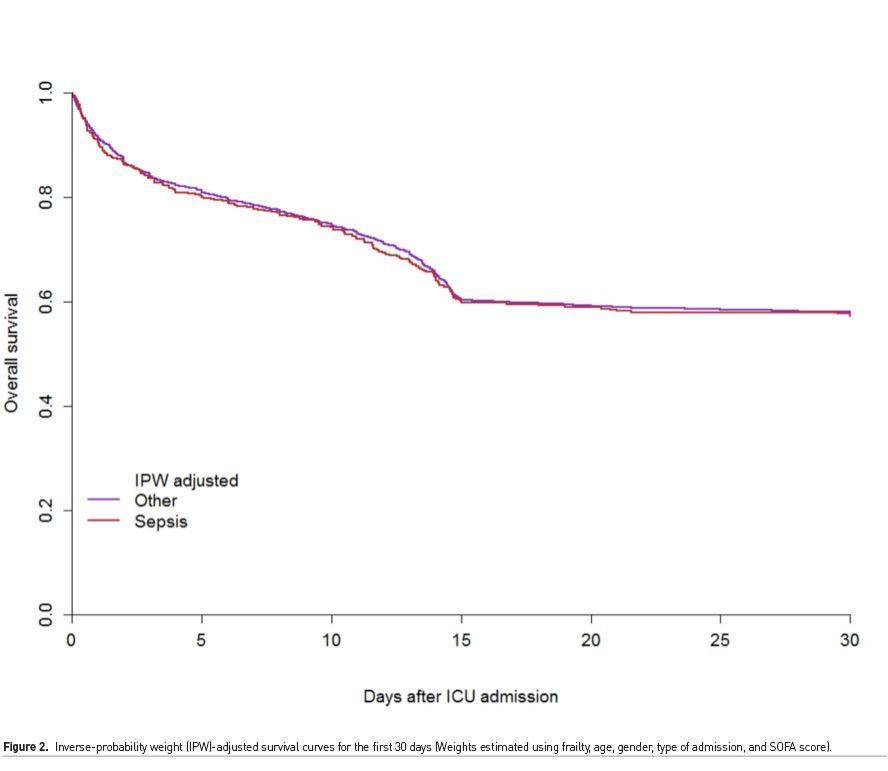
Our main research question was to analyse if sepsis was a determinant factor for outcome in VIPs admitted to the ICU with the diagnosis of sepsis and secondly, to identify risk factors for 30-day mortality. Hence, we compared patients admitted for sepsis (suspected or demonstrated focus of infection and SOFA score ≥ 2) with the patients admitted for any other acute reason. Of 3869 acutely admitted VIPs, 493 (12.7%) were admitted for sepsis; 54% were male, median age was 83 and medium SOFA score was 9. Frailty was present in 54%. ICU and 30-day mortality were 28.4% and 42% respectively, similar to other acute patients. Sepsis had no impact on 30-day survival [HR 0.99 (95% CI 0.86–1.15), p = 0.917]. Inverse-probability weight (IPW)-adjusted survival curves for the first 30 days after ICU admission were similar for acute septic and non-septic patients [HR: 1.00 (95% CI 0.87–1.17), p = 0.95] (Figure 2). Age, frailty and SOFA score were the independent factors associated with 30-day survival in all acute VIPs with SOFA≥2. In a recent study on 532 septic patients from 3596 acute very old patients admitted in the ICU, the same independent factors and not sepsis were significantly associated with 6-months mortality (Haas et al. 2021). Therefore, from our point of view, sepsis diagnosis should not be a factor to limit ICU admission in this old population.
Medium and Long-Term Outcome
An increasing number of old patients survive sepsis treatment, and their care does not finish at hospital discharge. Emerging data suggest that sepsis survivors frequently experience long-term disability, worsening of chronic health conditions and new symptoms which cause frequent re-hospitalisations and enhance health care utilisation and costs (Martin et al. 2006; Iwashyna et al. 2010; Philipart et al. 2013). They are more likely to be discharged from hospital to a nursing home or alternative health care facility rather than to their home. Subsequent infections, cardiovascular events, acute renal failure, and aspiration are increased after hospitalisation for sepsis.
There is an urgent need to improve management of these vulnerable old patients after hospital discharge. A multidisciplinary care is needed to optimise recovery and assure an adequate quality of life, both for the patient and relatives. In addition to that, as frailty usually increases with age, readmissions should be carefully considered, and palliative care-related decisions should be defined. Special attention should be paid to the medications. Frequently, the ones administered while they are at hospital are continued at home and most of them are not necessary and cause sleep cycle alterations, memory loss, and lack of attention mainly with hypnotics and antipsychotics.
Conclusion
Our population is ageing and although they can be in a particularly good condition in their usual life, an acute insult can be decisive in their outcome. The challenge is the ability for an early sepsis detection, resuscitation, antibiotic administration, and drainage of septic focus if necessary. Frailty and disease severity, not just age or clinical diagnosis, should help to guide triage. The goal of treatment and patient’s wishes should be honestly discussed. Failure to respond to treatment should be followed by reassuring comfort to the patient and support to his family. Finally, further research is required regarding the care of very elderly patients who have survived sepsis.
After all these thoughts and regarding the patient I saw in the emergency room; I think he probably had a sepsis from a urinary tract infection. Given that my patient is not frail, his comorbidities are well controlled and urinary sepsis has a good prognosis in very old patients, I should admit him to the ICU and give him the chance to recover from his sepsis
Conflict of Interest
None.
References:
Angus DC, Linde-Zwirble WT, Lidicker J et al. (2001) Epidemiology of severe sepsis in the United States: Analysis of incidence, outcome, and associated costs of care. Crit Care Med, 29:1303–10.
Clegg A, Young J, Iliffe S et al. (2013) Frailty in elderly people. Lancet, 381:752–62.
Dugani S, Veillard J, Kissoon N (2008) Reducing the global burden of sepsis. CMAJ, 9;189(1): E2-E3, doi: 10.1503/cmaj.160798.
Fabri A, Marchesini G, Benazzi B et al. (2019) Old subjects with sepsis in the emergency department: trend analysis of case fatality rate. BMC Geriatrics, 19:372. doi.org/10.1186/s12877-019-1384-8
Fernando SM, McIsaac DI, Perry JJ et al. (2019) Frailty and Associated Outcomes and Resource Utilization Among Older ICU Patients With Suspected Infection. Crit Care Med, 47(8): e669-e676, doi.org/10.1097/ccm.0000000000003831.
Ferrer R, Artigas A, Levy MM et al. (2008) Improvement in process of care and outcome after a multicenter severe sepsis educational program in Spain. JAMA, 299:2294–303.
Flatten H, de Lange DW, Artigas A et al. (2017) The status of intensive care medicine research and a future agenda for very old patients in the ICU. Intensive Care Med, 43:1319–28.
Flaatten H, De Lange DW, Morandi A et al. (2017) The impact of frailty on ICU and 30-day mortality and the level of care in very elderly patients (≥ 80 years). Intensive Care Med, 43:1820–8.
Fleischmann C, Scherag A, Adhikari NK et al. (2016) Assessment of global incidence and mortality of hospital-treated sepsis. Current estimates and limitations. Am J Respir Crit Care Med, 193(3):259–72.
Guidet B, de Lange DW, Boumendil A et al. (2020) The contribution of frailty, cognition, activity of daily life and comorbidities on outcome in acutely admitted patients over 80 years in European ICUs: the VIP2 study. Intensive Care Med, 46:57-69.
Haas LEM, Van Dillen LS, de Lange DW, et al. (2017) Outcome of very old patients admitted to the ICU for sepsis: a systematic review. Eur Geriatr Med, 8:446–53.
Ibarz M, Boumendil A, Haas LEM et al. (2020) Sepsis at ICU admission does not decrease 30 day survival in very old patients: a post-hoc analysis of the VIP1 multinational cohort study. Ann Intensive Care, 10:56, doi.org/10.1186/s13613-020-00672-w
Iwashyna TJ, Ely EW, Smith DM, Langa KM (2010) Long-term Cognitive Impairment and Functional Disability Among Survivors of Severe Sepsis. JAMA, 304:1787-94.
Kerckhoffs MC, Senekal J, van Dijk D et al. (2020) Framework to Support the Process of Decision Making on Life-Sustaining Treatments in the ICU: Results of a Delphi Study. Crit Care Med, 48(5):645-53.
Kotfis K, Wittebole X, Jaschinski U et al. (2019) A worldwide perspective of sepsis epidemiology and survival according to age: Observational data from the ICON audit. J Crit Care, 51: 122-32.
Lang PO, Mitchell WA, Lapenna A et al. (2010) Immunological pathogenesis of main-related diseases and frailty: role of immunosenescence. Eur Geriatr Med, 1:12-21.
Lee SH, Hsu TC, Lee MG et al. (2018) Nationwide trend of Sepsis: a comparison among octogenarians, elderly, and young adults. Crit Care Med, 46:926–34.
Levy MM, Evans LE, Rhodes A (2018) The Surviving Sepsis Campaign Bundle: 2018 Update. Crit Care Med, 46 (6):997-1000.
Martin GS, Mannino DM, Moss M (2006) The effect of age on the development and outcome of adult sepsis. Crit Care Med, 34:15–21.
Martin Loeches I, Guia MC, Vallecoccia MS et al. (2019) Risk factors for mortality in elderly and very elderly critically ill patients with sepsis: a prospective, observational, multicenter cohort study. Ann Intensive Care, 9:26-34. doi.org/10.1186/s13613-019-0495-x
Philippart F, Vesin A, Bruel C et al. (2013) The ETHICA study (part I): elderly’s thoughts about intensive care unit admission for life-sustaining treatments. Intensive Care Med, 39:1565–73.
Reinhart K, Daniels R, Kissoon N, Machado FR et al. (2017) Recognizing sepsis as a global health priority—a WHO resolution. N Engl J Med, 377 (5):414–7.
Rhodes A, Evans L, Alhazzani W et al. (2017) Surviving sepsis campaign: International guidelines for management of sepsis and septic shock. Crit Care Med, 45:486–552
Rockwood K, Song X, MacKnight C et al. (2005) A global clinical measure of fitness and frailty in elderly people. CMAJ, 173:489–95.
Rudd KE, Johnson SC, Agesa KM, Shackelford KA et al. (2020) Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet, 395(10219): 200–11.
Seymour CW, Gesten F, Prescott HC et al. (2017) Time to treatment and mortality during mandated emergency care for sepsis. N Engl J Med, 376:2235–44.
Singer M, Deutschman CS, Seymour CW et al. (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA, 315 (8):801–10.
Yébenes JC, Ruiz Rodriguez JC, Ferrer R et al. (2017) Epidemiology of sepsis in Catalonia: analysis of incidence and outcomes in a European setting. Ann Intensive Care, 7:19, doi.org/10.1186/s13613-017-0241-1





















