ICU Management & Practice, Volume 17 - Issue 2, 2017
Cardiac arrest (CA) causes ischaemic brain injury and persistent cerebral hypoperfusion and cerebral hypoxia during the early post-resuscitation period. PaCO2 is the major physiological regulator of cerebral blood flow, is a modifiable component of care and mild hypercapnia may lead to improved neurological outcomes for resuscitated CA survivors. In order to evaluate the potential therapeutic role of PaCO2, we will conduct the TAME Cardiac Arrest trial. If TTMH therapy, which is cost free, is shown to be effective, the lives of countless CA survivors will be improved, clinical practice will be transformed, and major financial and human cost savings will be realised.
Out-of-hospital cardiac arrest (OHCA) is a common, catastrophic event that represents a major public health problem around the world. In Australia, estimates of the incidence of OHCA are approximately 1 per 1,000 persons per year (approximately 25,000 individuals in Australia each year), with Australian mortality rates varying between 87 to 94% (Berdowski et al. 2010; Victorian Ambulance Cardiac Arrest Registry 2014). For resuscitated CA patients admitted to the Intensive Care Unit (ICU), devastating neurological injury leading to withdrawal of life support or clinically important neurological impairment are the most common outcomes following CA (Lemiale et al. 2013). Accordingly, while the initial problem is cardiac in nature, after ICU admission the main reason for such dismal outcomes is neurological injury. Thus a better neurological outcome is the logical and dominant therapeutic goal in this population (Schneider et al. 2013).
Previously, from a large, multicentre, retrospective observational study we reported the association of early PaCO2 values (first 24 hours) with clinical outcomes in 16,542 CA patients admitted to 125 Australia and New Zealand ICUs between 2000 and 2011 (Schneider et al. 2013). Our findings demonstrated that the occurrence of hypocapnia (PaCO2 <35 mmHg) carried a higher mortality rate and a lower likelihood of discharge home for survivors compared with normocapnia (PaCO2 35-45 mmHg). In contrast, hypercapnia (PaCO2 >45 mmHg) was independently associated with a 16% increase in the likelihood that a CA survivor would be discharged home, thus suggesting both safety and potential neurological benefit. Other subsequent observational studies involving adult resuscitated CA patients admitted to ICU indicate that hypercapnia is independently associated with improved neurological outcomes among survivors, while hypocapnia is associated with worse neurological outcomes, thus providing further evidence of the likely safety and possible benefit of hypercapnia (Eastwood et al. 2014; Vaahersalo et al. 2014).
Cerebral Perfusion and Arterial Carbon Dioxide Following Cardiac Arrest
It is well understood that CA leads to immediate brain ischaemia and that resuscitation leads to reperfusion injury with acute neuronal damage (Wiklund et al. 2012). What is underappreciated is that a state of sustained cerebral hypoperfusion develops and persists even after successful immediate resuscitation, return of spontaneous circulation (ROSC), and admission to the ICU (Ahn et al. 2014; Buunk et al. 2000; Koch et al. 1984). In this regard, several investigations using technologies like positron emission tomography (Edgren et al. 2003), middle cerebral artery blood flow assessment via Doppler ultrasound (Sundgreen et al. 2001), jugular bulb oxygen saturation (Buunk et al. 1999) and cerebral oximetry (Storm et al. 2014), all consistently show sustained hypoperfusion and cerebral hypoxia. For example, observational studies measuring cerebral tissue oxygen saturation (SctO2) by near-infrared spectroscopy in patients receiving post-resuscitation care have demonstrated persistent cerebral under-oxygenation and a statistically significant association between such lower SctO2 values and higher mortality rates (Ahn et al. 2014).
A likely pathophysiological mechanism responsible for such sustained early hypoperfusion relates to impaired cerebrovascular auto-regulation (Kock et al 1984; Sundgreen et al. 2001). Such impaired auto-regulation may, in turn, make even a normal arterial carbon dioxide tension (PaCO2) insufficient to achieve and maintain adequate cerebral perfusion and, consequently, cerebral oxygenation. However, PaCO2 is the major determinant of cerebral blood flow in humans (Curley et al. 2010; O’Croinin et al. 2005), and an increase in PaCO2 (hypercapnia) markedly increases cerebral blood flow under normal physiological conditions (Curley et al. 2010). The rapid vasodilatory effect of hypercapnia appears related to changes in arterial pH and cerebral vascular resistance (Koch et al. 1984; Meng & Gelb 2015). Additionally, elevated PaCO2 levels are known to have anti-convulsive, anti-inflammatory and antioxidant properties, which may attenuate the inflammatory component of reperfusion injury (Kavanagh and Laffey, 2006; Tolner et al. 2011). Conversely, hypocapnia is known to increase neuronal excitability, increase cerebral oxygen consumption, reduce cerebral blood flow and, thereby, potentially worsen reperfusion injury.
Crucially, PaCO2 is an easily modifiable variable and therefore a potential therapeutic target for the maintenance of cerebral perfusion and oxygenation in resuscitated CA patients (Schneider et al. 2013).
Cerebral Oxygenation and the Potential Role of Targeted Mild Hypercapnia
Until recently, there was no direct evidence on the effect of targeted hypercapnia on cerebral oxygenation in resuscitated CA patients to provide the additional biological rationale for its therapeutic application. To address this, we investigated the impact of targeted mild hypercapnia on cerebral oxygenation by performing a prospective double crossover physiological clinical study (Eastwood et al. 2016a). We enrolled seven adult resuscitated CA patients within 36 hours of their CA and compared the effect of targeting mild hypercapnia (PaCO2 50-55 mmHg) to standard care (TN) (PaCO2 35-45 mmHg) on regional SctO2. With a median time from CA to ROSC of 28 minutes, at a median of 26 hours 30 minutes after CA, during TN (a median PaCO2 of 37 mmHg), the median right and left frontal lobe SctO2 was low with a significant proportion of values clearly below normal. However, during targeted mild hypercapnia (a median PaCO2 of 52 mmHg), the median SctO2 had increased to normal or above normal. Such increases were substantial in magnitude and reliably occurred in every patient every time and were not associated with any adverse events. Such findings provide further evidence for the potential role of targeting mild hypercapnia to safely improve cerebral oxygenation.
Targeted Therapeutic Mild Hypercapnia After Cardiac Arrest
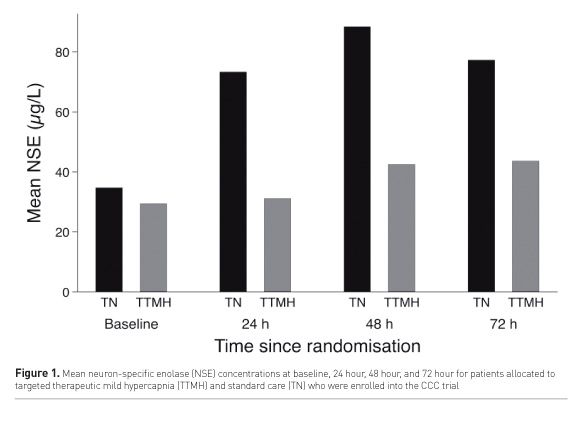
In late 2015, we completed a randomised, controlled, parallel group, multicentre, phase II trial (Eastwood et al. 2016b). This phase II trial sought to determine the preliminary biological efficacy, feasibility, safety of delivering TTMH to resuscitated CA patients compared to standard care (TN) for the 24 hours following ICU admission. This study allocated patients to either TTMH (PaCO2 50-55 mmHg) or standard care (TN) (PaCO2 35-45 mmHg). These targets were deliberately established to avoid episodes of hypocapnia in both arms. In order to achieve a target of 50 patients with full assessment of serum neuron-specific enolase (NSE) levels (baseline, 24 hour, 48 hour and 72 hour), 86 patients were randomised from four ICUs in Australia and New Zealand. NSE is a biomarker of neuronal injury. NSE is released into the bloodstream after injury, with lower concentrations over the first 72 hours following CA indicative of decreased neuronal injury. Thus, lower levels of NSE are associated with improved neurological outcome (Calderon et al. 2014).
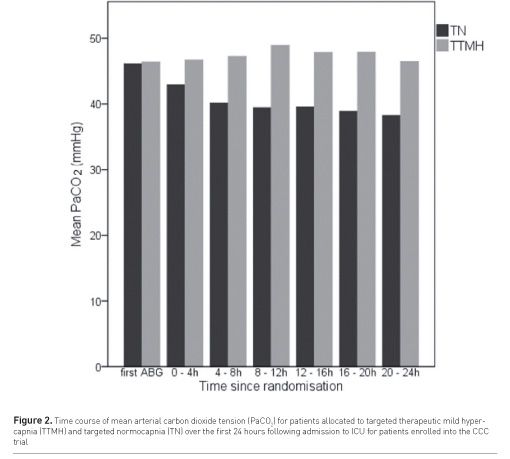
The study population had a median age of 61 years (79% male) and the majority were OHCA (78%). PaCO2 separation was achieved and sustained throughout the first 24 hours following randomisation (Figure 1). Overall, we found TTMH significantly attenuated NSE release compared with standard care (TN) over the first 72 hours (Figure 2), with an identical pattern for OHCA patients, thus providing a robust signal of biological efficacy for TTMH, without differences in ventilation, temperature, or sedation management. Importantly, patients allocated to either group both avoided episodes of hypocapnia or severe hypercapnia and no clinical adverse events, sudden neurological deterioration, or clinical signs of raised intracranial pressure were reported, supporting the safety of TTMH. Most importantly, at 6 months, overall 23 (59%) TTMH patients had improved neurological outcomes compared with 18 (46%) TN patients (Figure 3). In addition, hospital mortality occurred in 11 (26%) TTMH patients compared with 15 (37%) TN patients (p = 0.31)( Eastwood et al. 2016b).
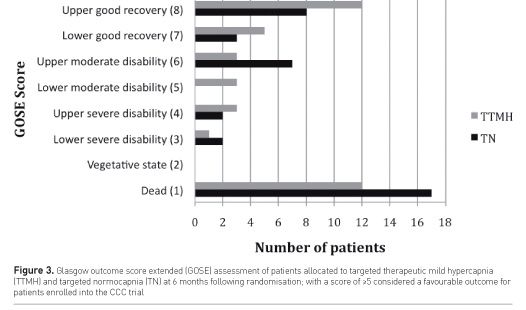
When the OHCA patients (80% of the cohort) were assessed separately, this effect was even stronger, as hospital mortality occurred in 8 (29%) TTMH patients compared with 13 (61%) TN patients. In addition, 20 (65%) TTMH patients had improved neurological outcomes compared with 16 (50%) TN patients (p=0.16). Thus, TTMH was associated with a beneficial biological effect (attenuated NSE levels) and a pattern of improved neurological and clinical outcomes (Eastwood et al. 2016b).
The TAME Cardiac Arrest Trial
There is now compelling epidemiological, biological, physiological, and supportive clinical data suggesting that TTMH can deliver significant outcome improvements in resuscitated CA patients admitted to ICU. In their aggregate, these findings strengthen the need to perform a larger phase III trial to address the question of whether TTMH improves patient-centred outcomes in resuscitated CA patients admitted to the ICU. As such, on behalf of the Australian Resuscitation Outcomes Consortium (Aus-ROC) NHMRC Centre of Research Excellence, the Australian New Zealand Intensive Care Society (ANZICS) Clinical Trials Group, and the Australian and New Zealand Intensive Care Research Centre (ANZIC-RC), the Targeted Therapeutic Mild Hypercapnia After Resuscitated Cardiac Arrest: A Phase III Multi-Centre Randomised Controlled Trial (The TAME Cardiac Arrest Trial) was developed. The primary outcome measure for this study will be the proportion of patients with a favourable neurological outcome at 6 months as assessed using the Glasgow Outcomes Scale Extended (GOSE) (defined as a score ≥5)(Wilson et al. 1998). Five key secondary outcomes include mortality, functional recovery, cognitive functional recovery, quality of life and a health economic evaluation.
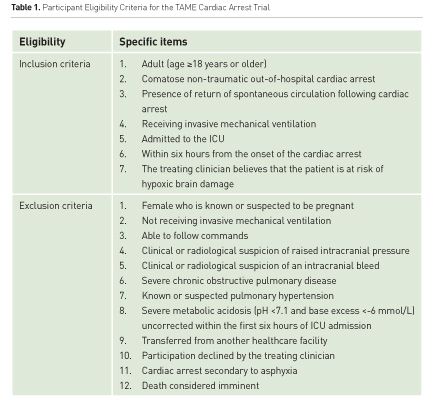
Briefly, the TAME Cardiac arrest trial will recruit 1,700 adult resuscitated OHCA patients from 30 ANZICS Clinical Trials Group member ICUs. All participating ICUs, stratified by site, will randomise patients via a website-enabled computer-generated code with permuted blocks. Eligibility criteria are shown in Table 1. Patients allocated to the TTMH protocol will be sedated to achieve moderate to deep sedation (a target Richmond Agitation Scale Score of –3 to –4). Arterial blood gases and end-tidal carbon dioxide levels will be measured at baseline and then used to guide respiratory rate adjustments of minute ventilation to remain within the target PaCO2 range of 50-55 mmHg. Arterial blood gases will be repeated every 4 hours for 24 hours following randomisation or if end-tidal carbon dioxide values change >5 mmHg. While patients allocated to the TN protocol will be managed according to current practice in Australia and New Zealand (Schneider et al. 2013) and in accordance with ILCOR guidelines, which recommend maintaining normocapnia in these patients (Neumar et al. 2010). For both groups, ventilation management for all patients will be guided by arterial blood gas data assessed after adjustment to 37oC (alpha-stat) (standard care) (Eastwood et al. 2015) and, to ensure safety, the treating ICU physician can modify patient management, including the use of sedative agents, muscle relaxants and paralysis, as clinically indicated throughout the 24-hour intervention period. Importantly, all pre-hospital and pre-ICU care will be performed in accordance with state/territory best practice guidelines and existing local protocols. In addition, all post-ICU patient management will be at the discretion of the patient’s ward-based treating physicians.
Conflict of interest
Glenn M. Eastwood declares that he has no conflict of interest. Rinaldo Bellomo declares that he has no conflict of interest.
Abbreviations
CA cardiac arrest
ICU intensive care unit
ILCOR International Liaison Committee on Resuscitation
NSE neuron-specific enolase
OHCA out-of-hospital cardiac arrest
PaCO2 arterial carbon dioxide tension
ROSC return of spontaneous circulation
SctO2 cerebral tissue oxygen saturation
TN targeted normocapnia
TTMH target therapeutic mild hypercapnia
References:
Ahn A, Yang J, Inigo-Santiago L et al. (2014) A feasibility study of cerebral oximetry monitoring during the post-resuscitation period in comatose patients. Resuscitation, 85: 522-6.
Berdowski J, Berg RA, Tijssen JG, et al. (2010) Global incidences of out-of-hospital cardiac arrest and survival rates: Systematic review of 67 prospective studies. Resuscitation, 81: 1479-87.
Buunk G, van der Hoeven JG, Meinders AE (1999) Prognostic significance of the difference between mixed venous and jugular bulb oxygen saturation. Resuscitation, 41: 257-62.
Calderon LM, Guyette FX, Doshi AA et al. (2014) Combining NSE and S100B with clinical examination findings to predict survival after resuscitation. Resuscitation, 85: 1025-9.
Curley G, Laffey JG, Kavanagh BP (2010) Bench-tobedside review: carbon dioxide. Crit Care, 14(2): 220.
Eastwood GM, Young PJ, Bellomo R (2014) The impact of oxygen and carbon dioxide management on outcome after cardiac arrest. Curr Opin Crit Care, 20: 266-72.
Eastwood GM, Suzuki S, Lluch C, et al. (2015) A pilot assessment of alpha-stat vs pH-stat arterial blood gas analysis after cardiac arrest. J Crit Care, 30: 138-44.
Eastwood GM, Tanaka A, Bellomo R (2016) Cerebral oxygenation in mechanically ventilated early cardiac arrest survivors: The impact of hypercapnia. Resuscitation, 102: 11-16.
Eastwood GM, Schneider AG, Suzuki S et al. (2016) Targeted therapeutic mild hypercapnia after cardiac arrest: A phase II multi-centre randomised controlled trial (the CCC trial). Resuscitation, 104: 83-90.
Edgren E, Enblad P, Grenvik A et al. (2003)Cerebral blood flow and metabolism after cardiopulmonary resuscitation. A pathophysiologic and prognostic positron emission tomography pilot study. Resuscitation, 57: 161-70.
Kavanagh BP, Laffey JG (2006) Hypercapnia. Minerva Anestesiol, 72: 567-76.
Koch KA, Jackson DL, Schmiedl M et al. (1984) Total cerebral ischemia: effect of alterations in arterial PCO2 on cerebral microcirculation. J Cereb Blood Flow Metab, 4: 343-9.
Lemiale V, Dumas F, Mongardon N et al. (2013) Intensive care unit mortality after cardiac arrest. Intensive Care Med, 39: 1972-80.
Meng L, Gelb AW.(2015) Regulation of cerebral autoregulation by carbon dioxide. Anesthesiology, 122: 196-205.
Neumar RW, Otto CW, Link MS et al. (2010) Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation, 122: S729-67.
O’Croinin D. Ni Chonghaile M, Higgins B et al. (2005) Bench-to-bedside review: Permissive hypercapnia. Crit Care, 9: 51.
Schneider AG, Eastwood GM, Bellomo R et al. (2013) Arterial carbon dioxide tension and outcome in patients admitted to the intensive care unit after cardiac arrest. Resuscitation, 84: 927-34.
Storm C, Leithner C, Krannich A et al. (2014) Regional cerebral oxygen saturation after cardiac arrest in 60 patients--a prospective outcome study. Resuscitation, 85: 1037-41.
Sundgreen C, Larsen FS, Herzog TM et al. (2001) Autoregulation of cerebral blood flow in patients resuscitated from cardiac arrest. Stroke, 32: 128-32.
Tolner EA, Hochman DW, Hassinen P et al. (2011) Five percent CO2 is a potent, fast-acting inhalation anticonvulsant. Epilepsia, 52: 104-14.
Vaahersalo J, Bendel S, Reinikainen M et al. (2014) Arterial blood gas tensions after resuscitation from out-of-hospital cardiac arrest. Crit Care Med, 42: 1463-70.
Victorian Ambulance Cardiac Arrest Registry (2014) Victorian Ambulance Cardiac Arrest Registry annual report 2013-2014. Doncaster, VIC: Ambulance Victoria.
Wiklund L, Martijn C, Miclescu A et al. (2012) Central nervous tissue damage after hypoxia and reperfusion in conjunction with cardiac arrest. Int Rev Neurobiol, 102: 173-87.
Wilson JT, Pettigrew LE, Teasdale GM (1998) Structured interviews for the Glasgow Outcome Scale and the extended Glasgow Outcome Scale. J Neurotrauma, 15: 573-85.





















