ICU Management & Practice, Volume 19 - Issue 3, 2019
The EACTS/EACTA Guidelines on patient blood management for adult cardiac surgery.
The EACTS/EACTA guidelines were published jointly by the Society of Cardiothoracic Anesthesia and Cardiac Surgery for patient blood management. In the bleeding patient with a low fibrinogen level (<1.5 g/L), fibrinogen substitution may be considered to reduce postoperative bleeding and transfusions. However, the prerequisite is a bleeding patient. In patients where bleeding is related to coagulation factor deficiency, prothrombin complex concentrates (PCC), or fresh frozen plasma (FFP) administration should be considered to reduce bleeding and transfusions (Boer et al. 2017).
As far as clinical evidence is concerned, there is conflicting data with respect to fibrinogen supplementation. In a study conducted about four years ago, patients were randomised to receive either fibrinogen or placebo. This was a non-pragmatic trial conducted in an artificial environment where patients that had bleeding due to other reasons were excluded. The goal was to demonstrate that a first-line fibrinogen supplementation would avoid the need for FFP and would reduce the need for any kind of transfusions. The primary endpoint was achieved (Figure 1), and the group treated with fibrinogen had zero need for FFP or platelets (Ranucci et al. 2015).
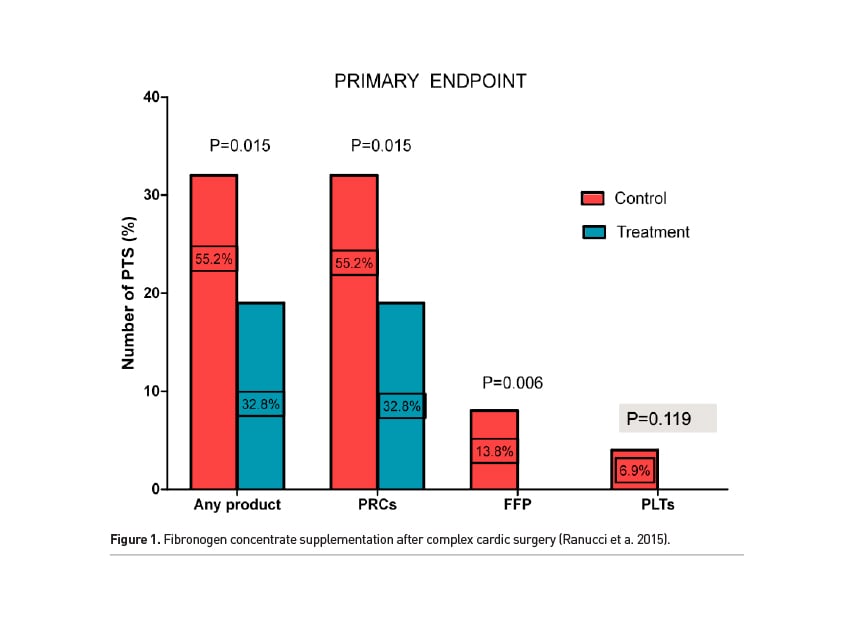
However, the Randomized Evaluation of Fibrinogen vs. Placebo in Complex Cardiovascular Surgery (REPLACE) study provided different results. Fibrinogen administration resulted in higher reduction of bleeding (Figure 2). Medication was administered to patients with a 5 minute bleeding mass of 60-250g after separation from bypass and surgical haemostasis. Study findings did not demonstrate a reduction in total units of allogenic blood products (ABP) [FFP, platelets, and/or RBCs] transfused over 24 hours with fibrinogen concentrate compared with placebo. Surprisingly, human fibrinogen concentrate was found to be associated with increased blood product transfusion compared to placebo (Rohe-Meyer N et al. 2016).
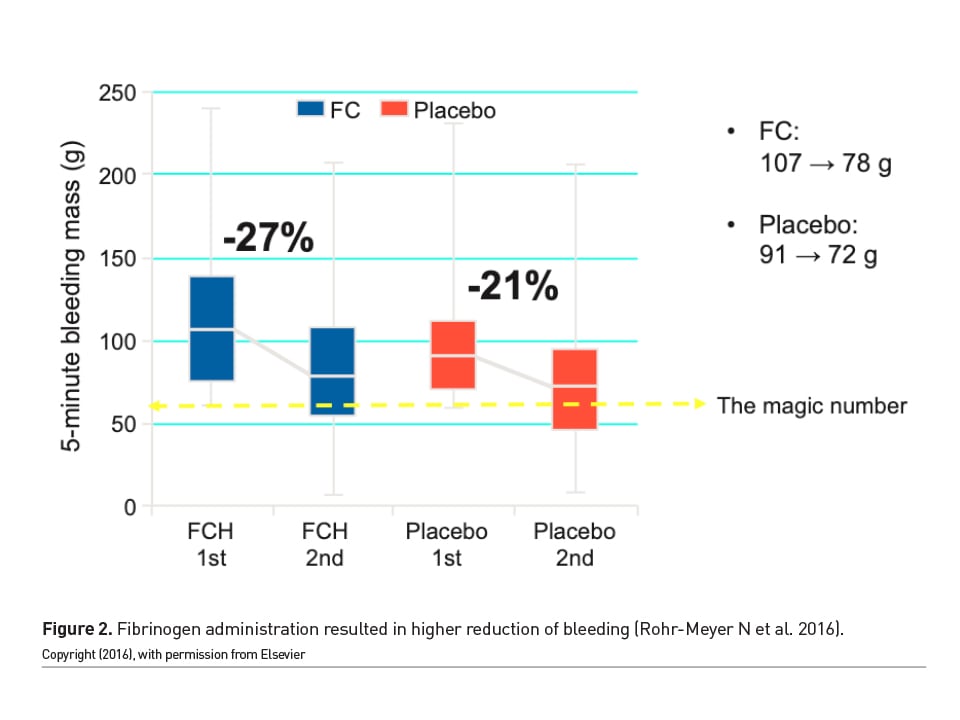
Yet another very well-designed study that focused on intraoperative bleeding showed different findings. Patients were randomised into two groups where they received an intravenous, single dose of fibrinogen concentrate or placebo. The primary outcome was blood loss between intervention and closure of chest. In patients with intraoperative bleeding during high-risk cardiac surgery, administration of fibrinogen concentrate resulted in no significant difference in the amount of intraoperative blood loss compared to placebo (Bilecen S. et al. 2017). There was one problem, however. The window of observation of bleeding was incredibly short. The observation time of bleeding was six minutes. The control group bled 70 millilitres and the study group 50 millilitres.
Blood, Blood Products And Derivatives - Use In Trauma And Cardiac/Liver Surgery
There are different solutions that are available for clinicians to reduce postoperative bleeding and transfusions. Here is a quick overview of the primary ones:
Fresh Frozen Plasma (FFP)
- Poor source of fibrinogen and prothrombin complexes
- Huge quantity needed
- Increasingly not considered the best product but still largely used
- Offers benefits whenever large volumes of fluids are required (e.g. in trauma patients)
- Very inexpensive
Cryoprecipitate
- Moderately good source of fibrinogen
- Limited volume overload
- Unavailable in many countries/hospitals but still largely used
- Multi-donor risks
- Probably will become less popular in the years to come
Prothrombin Complex Concentrate (PCCs)
- An elegant way to replace FFP
- Triggered by point-of-care haemostatic testing (POC) tests
- Associated with increased thromboembolic events and acute kidney injury (AKI)
- Effective but expensive
- Use likely to moderately increase in the years to come
Fibrinogen
- The main component of clot firmness
- Elegant way to replace FFP or cryoprecipitates
- Triggered by POC (mainly rotational thromboelastometry)
- Not associated with increased thromboembolic events
- Effective but expensive
- Dose unclear (both target concentration and dose calculation)
Therefore, to answer the question as to when to supplement with fibrinogen, the guidelines recommend that in the bleeding patient with a low fibrinogen level (<1.5 g/L), fibrinogen substitution may be considered to reduce postoperative bleeding and transfusions. In patients where bleeding is related to coagulation factor deficiency, PCC, or FFP administration should be considered to reduce bleeding and transfusions.
Key Points
- FFP is a poor source of fibrinogen and prothrombin complexes.
- Cryoprecipitate is a moderately good source of fibrinogen but has multi-donor risks.
- PCC and fibrinogen are both elegant ways to replace FFP.
- In the bleeding patient with a low fibrinogen level (<1.5 g/L), fibrinogen substitution may be considered to reduce postoperative bleeding and transfusions in bleeding patients with a low fibrinogen level.
- PCC or FFP administration should be considered to reduce bleeding and transfusions when bleeding is related to coagulation factor deficiency.
Abbreviations
ABC allogenic blood products
AKI acute kidney injury
FFP fresh frozen plasma
PCC prothrombin complex concentrates
PLT platelets
RBC red blood cells
References:
Bilecen S, de Groot JA, Kalkman CJ, Spanjersberg AJ, Brandon Bravo Bruinsma GJ, Moons KG, Nierich AP (2017) Effect of Fibrinogen Concentrate on Intraoperative Blood Loss Among Patients With Intraoperative Bleeding During High-Risk Cardiac Surgery: A Randomized Clinical Trial. JAMA,317(7):738-747.
Boer C, Meesters MI, Milojevic M, Benedetto U, Bolliger D, von Heymann C, Jeppsson A, Koster A, Osnabrugge RL, Ranucci M, Ravn HB, Vonk ABA, Wahba A, Pagano D (2018) 2017 EACTS/EACTA Guidelines on patient blood management for adult cardiac surgery. J Cardiothorac Vasc Anesth, 32(1):88-120.
Rahe-Meyer N, Levy JH, Mazer CD, Schramko A, Klein AA, Brat R, Okita Y, Ueda Y, Schmidt DS, Ranganath R, Gill R (2016) Randomized evaluation of fibrinogen vs. placebo in complex cardiovascular surgery (REPLACE): a double-blind phase III study of haemostatic therapy. Br J Anaesth, 117(1):41-51.
Ranucci M1, Baryshnikova E1, Crapelli GB1, Rahe-Meyer N2, Menicanti L3, Frigiola A3; Surgical Clinical Outcome Research (SCORE) Group (2015) Randomized, double-blinded, placebo-controlled trial of fibrinogen concentrate supplementation after complex cardiac surgery. J Am Heart Assoc, 2;4(6):e002066.




















