ICU Management & Practice, Volume 21 - Issue 5, 2021
What We Learned During the COVID-19 Pandemic That Should Not Be Forgotten
Introduction
Orotracheal intubation is a life-saving procedure in critically ill patients with acute respiratory failure, but complications during the procedure are frequent and life-threatening situations still occur in almost 45% of the procedures (Simpson et al. 2012; Russotto et al. 2021). The vast majority of clinical evidence on intubation is mainly focused on the operating room (OR). As opposed to traditional anatomical challenges, orotracheal intubation in the intensive care unit (ICU) imposes further risks due to the high prevalence of a physiological difficult airway (Mosier 2020).
The COVID-19 pandemic brought new challenges for intubation in the ICU. Severe respiratory failure and hypoxaemia, commonly present in COVID-19 patients, impose an increased risk of cardiovascular collapse and cardiac arrest during intubation. Besides, the procedure may expose healthcare professionals to contamination and changes in usual practice aiming at staff protection may unduly increase procedure difficulty (Feldman et al. 2020). Thus, while COVID-19 imposes challenges to intensive care physicians, it also creates opportunities for improvement in relation to intubation practices in the ICU.
Our objective with this piece is to summarise the available evidence about safe intubation practices in critically ill patients in light of new discoveries due to the coronavirus pandemic.
Intubation in Critically Ill Patients – Prior Evidence
Severe adverse events occur in 1 of 22.000 cases of orotracheal intubation in the operating room. On the other hand, the incidence of life-threatening complications may be as high as 45% during intubation in the ICU (Simpson et al. 2012; Russotto et al. 2021). It must be highlighted that this high incidence of complications in the ICU cannot be attributed solely to the lack of the anaesthesiologist. In a prospective comparison of intubation attempts for 208 patients intubated first in the OR and later in the ICU, both by anaesthesiologists, the incidence of difficult airway and complications were higher in the ICU, while first-time intubation success was lower when compared to the OR (Taboada et al. 2018). Intubation strategies – and risks – may vary among elective surgery and critically ill patients, but most of the clinical evidence is mainly focused on the OR.
The differences between airway management in the OR and ICU begins with the evaluation of the airway. Several predictors of difficult laryngoscopy, such as the 3-3-2 rule or the upper lip bite test depends on patient collaboration and may be unfeasible in the critically ill (Detsky et al. 2019). So far, the only validated airway assessment tool in ICU patients is the MACOCHA score, which still depends on the patient being able to sit for the Mallampati evaluation (De Jong et al. 2013). However, despite these limitations, assessing potential difficulties is advisable before all intubations in the ICU environment.
When it comes to efforts in preparing the scene to increase first attempt success, it is worth noting that the use of a checklist to ensure protocol adherence was not superior to standard care in a randomised controlled trial (Janz et al. 2018). Nevertheless, specific strategies during each step of the procedure can increase patient safety and must be implemented when possible.
Preparing the scene and patient positioning
Experienced staff is advisable for a safer procedure. Ideally, the presence of two airway operators with the presence of a senior physician can reduce the risk of overall complications (Schmidt et al. 2008). The leader must also plan and verbalise the primary and rescue strategies to be adopted to share their mental model with the team should any difficulties ensue during the procedure. Sedative agents, rescue devices and ventilation equipment must be checked and readily available. Two experienced operators and an easy access to a difficult airway trolley is advisable. One should not expect a bolus of fluid to be enough to manage hypotension or cardiovascular collapse. In a randomised controlled trial, routine infusion of a 500ml crystalloid solution did not prevent the occurrence of hypotension during intubation in the ICU in the absence of hypovolaemia (Janz et al. 2019). Therefore, norepinephrine must be readily available if hypotension is expected. Finally, sniff positioning must be optimal and is superior to other strategies of patient positioning during intubation in the ICU (Semler et al. 2017). Figure 1 exemplifies scene preparation before orotracheal intubation.
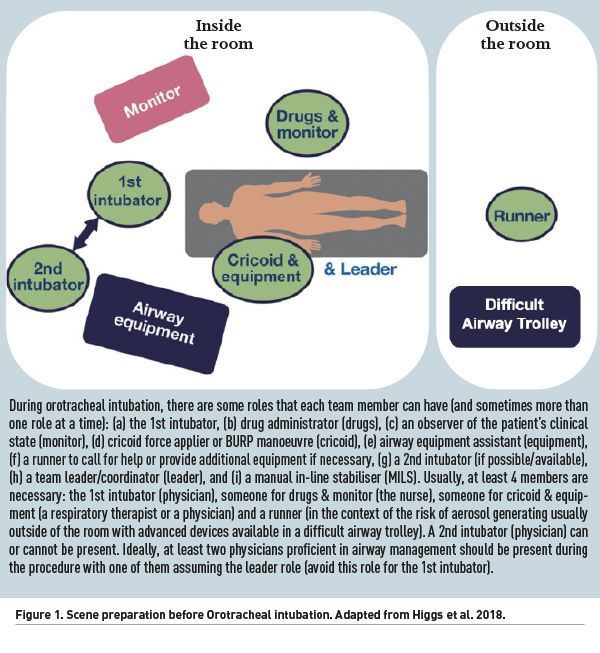
Pre-oxygenation
Pre-oxygenation before intubation aims at prolonging the period of safe apnoea after sedation and neuromuscular blockade. Offering 100% oxygen for 3 to 5 minutes reduces the risk of desaturation in comparison to standard of care. Strategies for proper pre-oxygenation includes the use of noninvasive ventilation, high-flow nasal canula, bag-valve-mask ventilation with 15 L/min oxygen and nonrebreather mask with a flush-rate oxygen delivery ( >40 L/min). A randomised controlled trial suggested that bag-valve mask ventilation before first intubation attempt improved patient oxygenation without an increased risk for aspiration of gastric content. Although not definitive, these results suggest that ventilation before intubation is not harmful as previously reported and may be interesting in severely hypoxaemic patients (Casey et al. 2019). On the other hand, apnoeic oxygenation during intubation with nasal catheter or high-flow nasal canula seems ineffective and should not be routinely performed (Vourc’h et al. 2015; Bailard et al. 2006; Simon et al. 2016; Semler et al. 2016).
Sedation strategies and use of neuromuscular blockade
There is not enough evidence to support the use of a specific sedation strategy over another during intubation in the ICU. In an observational cohort in 34 institutions, etomidate, propofol, midazolam and ketamine were the most used drugs by intensivists (Groth et al. 2018). The patient baseline condition is usually determinant in the choice of sedation strategy. Propofol and midazolam are more commonly used in a situation of haemodynamic stability, while etomidate and ketamine are preferred in a clinical scenario of shock (Mendes et al. 2020).
The use of neuromuscular blockade during intubation in the ICU is still a matter of debate. While several randomised controlled trials support the use of neuromuscular blockade and rapid sequence induction in the OR (Lundstrøm et al. 2018), the evidence in the ICU is based solely on observational studies (Li et al. 1999; Mosier et al. 2015; Wilcox et al. 2012). Potential risks of eliminating patient effort and respiratory drive with the use of NMB includes the risk of a rapid fall in patient oxygenation and a high risk of cardiovascular collapse in a do-not-intubate, do-not-ventilate scenario.
However, despite the lack of randomised trials and potential risks, available evidence suggests that the use of neuromuscular blockade can increase first attempt success and reduce overall complications during intubation in the ICU. So far, the use of NMB in the ICU may vary from 20 to 90% of intubations in different cohorts (Simpson et al. 2012; Yamanaka et al. 2010; Doig et al. 2009). In a recent survey regarding practices of airway management in the ICU, physicians reported the use of NMB in the minority of cases (Mendes et al. 2020).
Auxiliary devices and airway manipulation
Two recently published randomised controlled trials evaluated the use of auxiliary devices to increase first-attempt intubation success in the intensive care unit. The Styleto trial has shown that the routine use of a tracheal tube plus a stylet during intubation is superior to the tracheal tube alone to achieve first-attempt intubation success. Although this trial was not powered to evaluate possible differences among serious adverse events between groups, the use of a stylet did not increase traumatic injuries related to tracheal intubation in the ICU (Jaber et al. 2021). Similarly, a randomised trial evaluated the use of a bougie versus tracheal tube and stylet on first-attempt emergency intubation success. The rate of success was higher in the bougie group with similar rates of procedure related complications (Driver et al. 2018). Nevertheless, we believe adequate training about the caveats of using these devices is strongly advisable to avoid as much as possible preventable (and eventually fatal) complications associated with these devices, such as tracheal tears and posterior wall injuries, specially by inexperienced physicians.
When it comes to airway manipulation during intubation the most readily available strategy for dealing with difficult laryngoscopy is posterior displacement of the larynx by backward pression. The Sellick manoeuvre is largely adopted during intubation but it was originally described to “control regurgitation until intubation with a cuffed endotracheal tube was completed” and should not be the first strategy (Sellick 1961). On the contrary, the displacement of the larynx backward, upward and rightward with the so called BURP manoeuvre can improve vocal chords visualisation and may be adopted to improve intubation success (Takahata et al. 1997).
Direct laryngoscopy X Video laryngoscopy
Video laryngoscopy (VL) has emerged as a new standard of care or best practice during intubation in the ICU. It is supposed to provide a better view of the vocal cords even when difficulty is expected due to anatomical reasons. It does not demand a perfect alignment of the structures and can magnify the image, facilitating the intubation process. It also allows concurrent visualisation by a second operator that can immediately aid in airway management. However, it is more expensive and less available than direct laryngoscopy (DL). More important, previous knowledge of the intubation with DL is not directly transferrable to VL and variable learning curves can be expected.
In a small single center randomised trial, the use of VL improved first attempt success during urgent endotracheal intubation (Silverberg et al. 2015). However, in a larger trial published, VL compared with DL did not improve first attempt success rate and, unexpectedly, was associated with higher rates of severe life-threatening complications. The reasons for intubation failure varied among both strategies. In the DL group, the inability of glottis visualisation was the main reason for intubation failure. On the other hand, in the VL group, glottis visualisation was not possible in only 22% of the cases and failure of tracheal intubation was the most reported reason despite proper vocal cord visualisation. It is possible that the absence of previous training and proper skill may have contributed to the trial results (Lascarrou et al. 2017).
Confirmation of intubation
The use of waveform capnography to confirm intubation is mandatory and should not be considered as an optional auxiliary device. Lung auscultation and visualisation of chest wall movement are not reliable signs and cannot be used as single strategy to check intubation success, especially in the absence of neuromuscular blockade (Whitaker and Benson 2016; Linko et al. 1983).
The Need to Recognise and Anticipate the Physiologically Difficult Airway: A Life-Threatening Situation
As previously discussed, the occurrence of severe complications is much higher in the ICU setting than in the operating room. Cardiac arrest may occur in up to 4% of the patients and haemodynamic instability along with hypoxia are the most common reasons for this event (Russotto et al. 2021; Heffner et al. 2013). Moreover, life threatening situations may occur even with first attempt success in patients with severely deranged physiology and pre-intubation status is important to identify patients at increased risk for complications (Heffner et al. 2013). In a large retrospective cohort of intubation in critically ill patients, arterial hypotension prior to intubation, hypoxia prior to intubation, absence of pre-oxygenation,age and obesity were independently associated with cardiac arrest and death (De Jong et al. 2018). Three of these may be modifiable risk factors in case of proper recognition before initiating the procedure.
High-risk situations other than hypotension and hypoxaemia may also behave as physiologically difficult airway. Pulmonary hypertension or right ventricular dysfunction, severe acidosis, intracranial hypertension and the full stomach scenario may all impose a greater risk of complications, even in the absence of traditional anatomic predictors of difficult airway (Mosier 2020). Table 1 highlights physiologically difficult situations and possible strategies to overcome them.

Intubation in COVID-19 patients poses as a major challenge when it comes to physiologically difficult airway. Hypoxaemia is common and safe apnoea time may be as short as 60 seconds in lungs with a poor compliance (Mosier 2020). Moreover, the combination of severe hypoxaemia due to pneumonia and hypercapnia due to increased dead space ventilation further increases the risk of acute cor pulmonale and right ventricular dysfunction (Mekontso et al. 2016).

Intubation of the COVID-19 Respiratory Failure
Given that COVID-19 is a disease transmitted predominantly by droplets, intubation and airway management are procedures with high level of exposure of healthcare workers and increased risk of contracting the illness. Some proposed changes in usual practice due to the COVID-19 pandemic affected all steps of intubation, from preparation to checking proper tube position. Therefore, protective measures are important but may increase the risk of severe complications and it is necessary to balance the risks and benefits of each of these measures.
What has changed that increased the procedure risk
To reduce staff exposition, guidelines and recommendations suggested to limit the number of people inside the room (Cook et al. 2020; Orser 2020). However, previous publications also suggested that two operators can reduce complications during the procedure. Therefore, a reduced number of people is adequate but the presence of two airway operators is still advisable (Jaber et al. 2006). Also, initial recommendations suggested changes in patient preoxygenation to reduce staff exposure to aerosol. Non-invasive ventilation and high flow nasal canula were contraindicated by some (Cook et al. 2020). Moreover, low flow non-rebreathing mask, which is incapable of providing 100% oxygen, was suggested as a possible alternative. Although the concern with aerosolisation is understandable, poor preoxygenation can reduce the safe apnoea time and decrease first attempt success. Desperate rescue manoeuvres due to severe desaturation is probably more problematic than the use of proper preoxygenation, eventually leading to cardiac arrest and a crash scenario where any concerns about staff safety are forgotten. Another common reason for crashing after intubation is to forget about the necessary trade-off of increasing respiratory rates when using low tidal volume ventilation for acute hypoxaemic respiratory failure. This has been a frequent observation in our practice, especially with physicians inexperienced with a physiologically difficult airway. Finally, the use of bag mask ventilation and even the use of certain supraglottic devices were discouraged during intubation in COVID-19 patients. However, emergent surgical access of a failed first attempt is probably more difficult and riskier for the patient and staff than traditional algorithms in “do-not-intubate” situations (Brasileira 2020).
What has changed that improved patient safety
On the other hand, some recommendations during intubation in COVID-19 should come to stay as the new standard of practice in the ICU. The presence of a runner outside the room with an easy access to rescue devices is advisable and can accelerate the process of accessing an urgent or crashed airway. Moreover, COVID-19 has brought the best experienced airway manager to the patient room. In any intubation, even if a less experienced operator is primarily managing the airway, a senior staff must be present to ensure a low rate of complications (Cook et al. 2020). Despite initial recommendations, recent trials evaluating the use of noninvasive ventilation and high flow nasal canula in COVID-19 patients have facilitated personnel acceptance of using these resources during intubation (Grieco et al. 2021). Adequate preoxygenation with available devices, especially positive pressure ventilation, must remain as the gold standard in preparation for intubation. The routine use of neuromuscular blockade to reduce cough and aerosol dispersion brought the experience of the operating room into the ICU. Although not tested in a randomised trial, available evidence suggests that this strategy can increase first attempt success (Li et al. 1999; Mosier et al. 2015; Wilcox et al. 2012). Fnally, some have suggested a faster escalation to senior physicians and between devices (such as the adoption of the Vortex approach) instead of repeat attempts (3 or more) with the same operator and/or device. With adequate preparedness and sharing of the mental model of the most experienced physician, sharp decision-making during airway management is a desired consequence to improve procedural safety.
Current Approach to Airway Management - Suggested Do’s and Don’ts
In Table 2, we suggest current do’s and don’ts on airway management for critically ill patients, COVID-19 or not, based on current literature, and the authors’ previous and acquired experience during the pandemic.
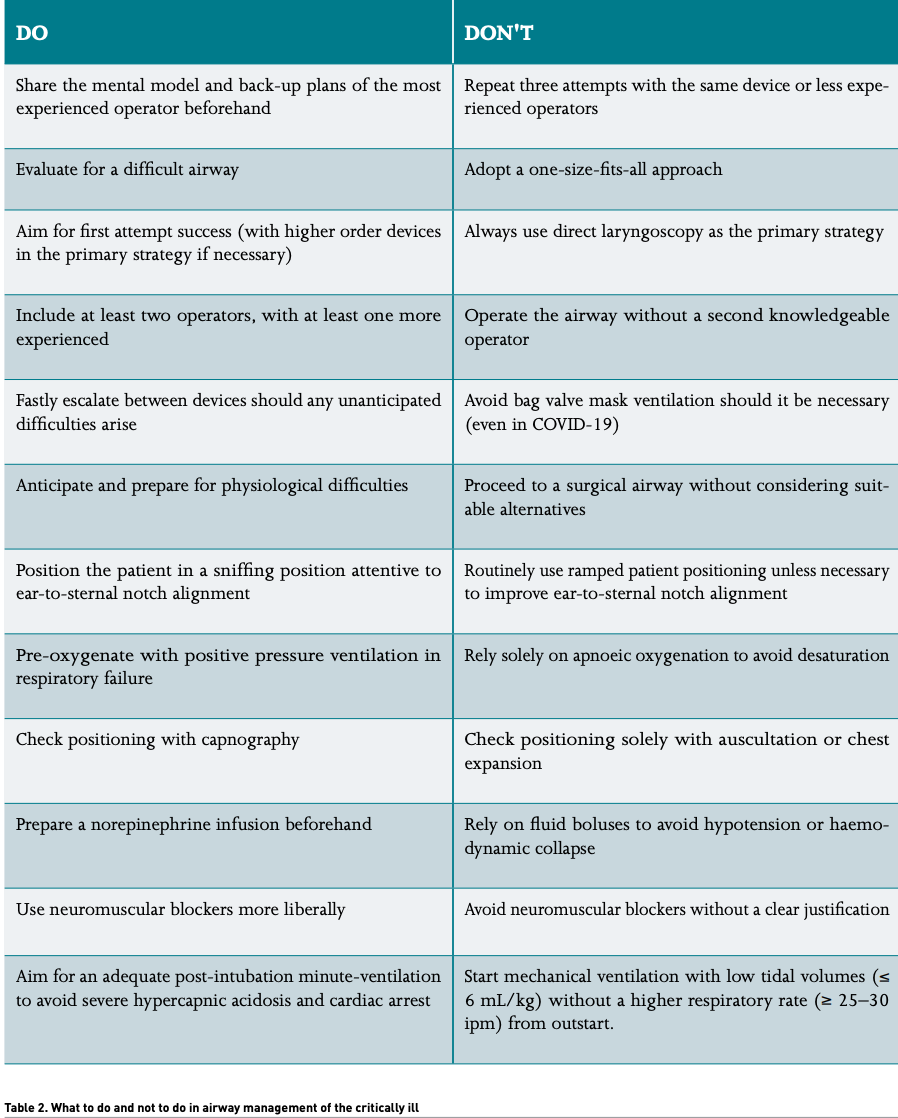
Conclusion
The COVID-19 pandemic brought several challenges to airway management practices in the ICU. The fear of staff contamination changed the usual practice with positive and negative effects to staff and patient safety. Now, after the experience with COVID-19 patients, it is important to filter which recommendations should be left aside and which ones must stay for good. As with other expert recommendations based on few observations that have led to suggestions of non-evidence informed approaches to the management of known syndromes in critically ill patients, we believe that airway management strategies should also have been maintained to current standards, actually taking them to higher standards if necessary. While protecting healthcare workers is a top priority (and should be done with proper protective equipment), lowering airway management standards for staff protection is both unacceptable and unadvisable. The main lesson we learned in airway management during the pandemic is to keep the highest possible standards informed by the best available evidence to avoid potentially catastrophic and lethal complications.
Conflict of Interest
None. 
References:
Baillard C, Fosse JP, Sebbane M et al. (2006) Noninvasive ventilation improves preoxygenation before intubation of hypoxic patients. Am J Respir Crit Care Med, 174(2):171-7.
Brasileira AdMI. Recomendações da Associação de Medicina Intensiva Brasileira para a abordagem do COVID-19 em medicina intensiva 2020. Available from: https://www.amib.org.br/fileadmin/user_upload/amib/2020/junho/10/Recomendacoes_AMIB-3a_atual.-10.06.pdf.
Casey JD, Janz DR, Russell DW et al. (2019) Bag-Mask Ventilation during Tracheal Intubation of Critically Ill Adults. N Engl J Med, 380(9):811-21.
Cook TM, El-Boghdadly K, McGuire B et al. (2020) Consensus guidelines for managing the airway in patients with COVID-19: Guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia, 75(6):785-99.
De Jong A, Molinari N, Terzi N et al. (2013) Early identification of patients at risk for difficult intubation in the intensive care unit: development and validation of the MACOCHA score in a multicenter cohort study. Am J Respir Crit Care Med, 187(8):832-9.
De Jong A, Rolle A, Molinari N et al. (2018) Cardiac Arrest and Mortality Related to Intubation Procedure in Critically Ill Adult Patients: A Multicenter Cohort Study. Crit Care Med, 46(4):532-9.
Detsky ME, Jivraj N, Adhikari NK et al. (2019) Will This Patient Be Difficult to Intubate?: The Rational Clinical Examination Systematic Review. JAMA, 321(5):493-503.
Doig GS, Heighes PT, Simpson F et al. (2009) Early enteral nutrition, provided within 24 h of injury or intensive care unit admission, significantly reduces mortality in critically ill patients: a meta-analysis of randomised controlled trials. Intensive Care Med, 35(12):2018-27.
Driver BE, Prekker ME, Klein LR et al. (2018) Effect of Use of a Bougie vs Endotracheal Tube and Stylet on First-Attempt Intubation Success Among Patients With Difficult Airways Undergoing Emergency Intubation: A Randomized Clinical Trial. JAMA, 319(21):2179-89.
Feldman O, Meir M, Shavit D et al. (2020) Exposure to a Surrogate Measure of Contamination From Simulated Patients by Emergency Department Personnel Wearing Personal Protective Equipment. JAMA, 323(20):2091-3.
Grieco DL, Menga LS, Cesarano M et al. (2021) Effect of Helmet Noninvasive Ventilation vs High-Flow Nasal Oxygen on Days Free of Respiratory Support in Patients With COVID-19 and Moderate to Severe Hypoxemic Respiratory Failure: The HENIVOT Randomized Clinical Trial. JAMA, 325(17):1731-43.
Groth CM, Acquisto NM, Khadem T (2018) Current practices and safety of medication use during rapid sequence intubation. J Crit Care, 45:65-70.
Heffner AC, Swords DS, Neale MN, Jones AE (2013) Incidence and factors associated with cardiac arrest complicating emergency airway management. Resuscitation, 84(11):1500-4.
Higgs A, McGrath BA, Goddard C et al. (2018) Guidelines for the management of tracheal intubation in critically ill adults. Br J Anaesth, 20(2):323-52.
Jaber S, Rollé A, Godet T et al. (2021) Effect of the use of an endotracheal tube and stylet versus an endotracheal tube alone on first-attempt intubation success: a multicentre, randomised clinical trial in 999 patients. Intensive Care Med, 47(6):653-64.
Jaber S, Amraoui J, Lefrant JY et al. (2006) Clinical practice and risk factors for immediate complications of endotracheal intubation in the intensive care unit: a prospective, multiple-center study. Crit Care Med, 34(9):2355-61.
Janz DR, Semler MW, Joffe AM et al. (2018) A Multicenter Randomized Trial of a Checklist for Endotracheal Intubation of Critically Ill Adults. Chest, 153(4):816-24.
Janz DR, Casey JD, Semler MW et al. (2019) Effect of a fluid bolus on cardiovascular collapse among critically ill adults undergoing tracheal intubation (PrePARE): a randomised controlled trial. Lancet Respir Med, 7(12):1039-47.
Lascarrou JB, Boisrame-Helms J, Bailly A et al. (2017) Video Laryngoscopy vs Direct Laryngoscopy on Successful First-Pass Orotracheal Intubation Among ICU Patients: A Randomized Clinical Trial. JAMA, 317(5):483-93.
Li J, Murphy-Lavoie H, Bugas C et al. (1999) Complications of emergency intubation with and without paralysis. Am J Emerg Med, 17(2):141-3.
Linko K, Paloheimo M, Tammisto T (1983) Capnography for detection of accidental oesophageal intubation. Acta Anaesthesiol Scand, 27(3):199-202.
Lundstrøm LH, Duez CHV, Nørskov AK et al. (2018) Effects of avoidance or use of neuromuscular blocking agents on outcomes in tracheal intubation: a Cochrane systematic review. Br J Anaesth, 120(6):1381-93.
Mekontso Dessap A, Boissier F, Charron C et al. (2016) Acute cor pulmonale during protective ventilation for acute respiratory distress syndrome: prevalence, predictors, and clinical impact. Intensive Care Med, 42(5):862-70.
Mendes PV, Besen BAMP, Lacerda FH et al. (2020) Neuromuscular blockade and airway management during endotracheal intubation in Brazilian intensive care units: a national survey. Rev Bras Ter Intensiva, 32(3):433-8.
Mosier JM (2020) Physiologically difficult airway in critically ill patients: winning the race between haemoglobin desaturation and tracheal intubation. Br J Anaesth, 125(1):e1-e4.
Mosier JM, Sakles JC, Stolz U et al. (2015) Neuromuscular blockade improves first-attempt success for intubation in the intensive care unit. A propensity matched analysis. Ann Am Thorac Soc, 12(5):734-41.
Orser BA (2020) Recommendations for Endotracheal Intubation of COVID-19 Patients. Anesth Analg, 130(5):1109-10.
Russotto V, Myatra SN, Laffey JG et al. (2021) Intubation Practices and Adverse Peri-intubation Events in Critically Ill Patients From 29 Countries. JAMA, 325(12):1164-72.
Schmidt UH, Kumwilaisak K, Bittner E et al. (2008) Effects of supervision by attending anesthesiologists on complications of emergency tracheal intubation. Anesthesiology, 109(6):973-7.
Sellick BA (1961) Cricoid pressure to control regurgitation of stomach contents during induction of anaesthesia. Lancet, 2(7199):404-6.
Semler MW, Janz DR, Russell DW et al. (2017) A Multicenter, Randomized Trial of Ramped Position vs Sniffing Position During Endotracheal Intubation of Critically Ill Adults. Chest, 152(4):712-22.
Semler MW, Janz DR, Lentz RJ et al. (2016) Randomized Trial of Apneic Oxygenation during Endotracheal Intubation of the Critically Ill. Am J Respir Crit Care Med, 193(3):273-80.
Silverberg MJ, Li N, Acquah SO, Kory PD (2015) Comparison of video laryngoscopy versus direct laryngoscopy during urgent endotracheal intubation: a randomized controlled trial. Crit Care Med, 43(3):636-41.
Simon M, Wachs C, Braune S et al. (2016) High-Flow Nasal Cannula Versus Bag-Valve-Mask for Preoxygenation Before Intubation in Subjects With Hypoxemic Respiratory Failure. Respir Care, 61(9):1160-7.
Simpson GD, Ross MJ, McKeown DW, Ray DC (2012) Tracheal intubation in the critically ill: a multi-centre national study of practice and complications. Br J Anaesth, 108(5):792-9.
Taboada M, Doldan P, Calvo A et al. (2018) Comparison of Tracheal Intubation Conditions in Operating Room and Intensive Care Unit: A Prospective, Observational Study. Anesthesiology, 129(2):321-8.
Takahata O, Kubota M, Mamiya K et al. (1997) The efficacy of the "BURP" maneuver during a difficult laryngoscopy. Anesth Analg, 84(2):419-21.
Vourc'h M, Asfar P, Volteau C et al. (2015) Bachoumas K, Clavieras N, Egreteau PY, et al. High-flow nasal cannula oxygen during endotracheal intubation in hypoxemic patients: a randomized controlled clinical trial. Intensive Care Med, 41(9):1538-48.
Whitaker DK, Benson JP (2016) Capnography standards for outside the operating room. Curr Opin Anaesthesiol, 29(4):485-92.
Wilcox SR, Bittner EA, Elmer J et al. (2012) Neuromuscular blocking agent administration for emergent tracheal intubation is associated with decreased prevalence of procedure-related complications. Crit Care Med, 40(6):1808-13.
Yamanaka CS, Góis AF, Vieira PC et al. (2010), Orotracheal intubation: physicians knowledge assessment and clinical practices in intensive care units. Rev Bras Ter Intensiva, 22(2):103-11.






















