HealthManagement, Volume 22 - Issue 2, 2022
New Clinical Pathways for Parkinson’s Patients
Key Points
- There is a major systematic gap in what is on offer in terms of rehabilitation to patients with Parkinson’s disease.
- vCare combines an individualised clinical pathway, that has been activated by a clinician, with a holistic approach; a smart home installation that uses sensors; and a virtual coach.
- vCare’s immediate step is to exploit more proactively the benefits it has for the rehabilitation of people with Parkinson’s, such as improving their general quality of life, cognitive and motor improvement, and better patient adherence to rehabilitation, among others.
How to offer ongoing and sustained rehabilitation to patients’ who require it? Today, there is a major systematic gap in terms of what is on offer in terms of rehabilitation. vCare focuses on handling the gap in the current discontinuity of care in available forms of institutional care. The vCare system aims to help. It concentrates on patients who experience several mental and physical conditions: one of them is Parkinson’s disease. This article examines what the vCare system has to offer people with Parkinson’s.
- The vCare system has much to offer patients with Parkinson’s when they undergo rehabilitation.
- Between 50-80% of people with Parkinson’s experience motor difficulties 5-10 years into their experience of the condition. Over half of people with Parkinson’s eventually experience some level of dementia.
- vCare combines an individualised clinical pathway, that has been activated by a clinician, with a holistic approach; a smart home installation that uses sensors; and a virtual coach. The holistic approach covers a patient’s medical, social, cognitive, and other needs. The coach/avatar is supported by the use of both fixed rules and machine learning.
- Using experiences in the Basque Country in Spain, vCare has already shown there to be great benefits for people with Parkinson’s.
- vCare’s immediate step is to exploit more proactively the benefits it has for the rehabilitation of people with Parkinson’s, such as improving their general quality of life, cognitive and motor improvement, and better patient adherence to rehabilitation, among others. Its next step is to demonstrate the benefits of the solution through a large-scale clinical trial.
Secondary prevention is an essential element of long-term rehabilitation. To improve this situation, strategies oriented towards risk reduction, treatment adherence, and the optimisation of quality of life need to be developed. Frail and sometimes isolated patients often fail to adhere to the proposed post-discharge clinical path due to a lack of appropriate clinical, emotional and informational support. A recent literature review has demonstrated that virtual coaching systems are still rarely used to support secondary prevention in this context. The proposed vCare service contributes both to the shift from hospital-based to home-based rehabilitation and aims to fill an existing gap well identified by the medical community. This article focuses on the vCare design of a clinical pathway, by using the specific example of Parkinson’s disease.
Introduction to Patients with Parkinson’s Disease
Parkinson’s disease (Parkinson’s) affects 1.8% of people aged over 65 years and up to 5% of those above 85 years old in Europe. Parkinson’s is a slow, progressive disease, involving both motor and non-motor symptoms (Gómez-Esteban et al. 2007). The motor symptoms include slow movement, tremor/rigidity, and gait impairment. The non-motor symptoms cover cognitive impairment, neuropsychiatric symptoms, autonomic dysfunction, sleep disorders, constipation and urinary disturbances (Del Pino et al. 2021; Gómez-Esteban et al. 2011; Somme et al. 2015). Parkinson’s is the second most prevalent neurodegenerative disease after Alzheimer’s disease. Many of the symptoms are difficult for clinicians to monitor since they usually appear and get worse when a person is at home and/or during the night.
A group of clinicians based in the Basque Country in Spain (the Neurodegenerative diseases group at Biocruces Bizkaia Health Research Institute) has a particular interest in rehabilitation treatments that can be offered to patients with Parkinson’s. The group has explored potential changes in rehabilitation that are taking place today. Given changing socio-economic conditions, these Basque neurologists have taken an in-depth look at improving rehabilitation in patients’ own homes. The group has drawn especially on the work of the vCare initiative, a European co-financed project that aims at providing a smart solution to active secondary prevention.
Physical and Cognitive Rehabilitation of Parkinson’s Patients is Often Overlooked
Between 50-80% of patients with Parkinson’s present motor complications (such as fluctuations and involuntary motor movements) around 5-10 years after the onset of the disease. The risk of developing dementia is up to six times greater in Parkinson’s patients than the prevalence rate in the general population. The risk of dementia increases in relation to Parkinson’s disease duration, the patient’s age and male gender. Indeed, more than 50% of Parkinson’s patients have dementia. Among Parkinson’s patients who do not have dementia, about 25-30% have a mild cognitive impairment (Aarsland et al. 2010; Emre 2003).
Due to today’s high prevalence of Parkinson’s and the current limitation of resources in the public health systems, the health-care provision offered is mostly based on patients’ attending standard clinical visits to a neurologist (1 or 2 times per year). The neurologist attends to the patient’s neurological status and controls his or her pharmacological regimen (covering both motor and neuropsychiatric symptoms). Yet, the neurologist does not treat other critical needs of the Parkinson’s patient – such as physical and cognitive rehabilitation, risk factor monitoring, or social support – which can be resource-intensive and require continued supervision.
Currently, there are no universal recommendations/medical guidelines available on how to create programmes for home rehabilitation for patients with Parkinson’s (most Parkinson’s patients are outpatients and do not require a hospital stay: this differentiates them from patients with other pathologies). Instead, vCare can offer patients with Parkinson’s overall maintenance of their conditions, thereby helping them to avoid risks and improve their functionality, autonomy, and quality of life. In addition, vCare can reach a large number of patients, which can help to reduce reliance on rehabilitation centres. (This is a great achievement that also affects the empowerment of the patient and the long-term stimulation of rehabilitation programmes.) Thus, the ultimate scope of this component of the vCare project is to maintain and enhance the effects of long-term rehabilitation in patients with Parkinson’s from a multidisciplinary perspective. A virtual coach, such as the one developed by the vCare system, offers patients a smart solution that can help to provide a personalised home rehabilitation plan. Designed according to the patients’ own condition and habits, vCare can enhance patients’ quality of life and empower patients in adopting a healthy lifestyle (Kyriazakos et al. 2020; Seregni et al. 2021).
A Design for a New Continuous Home-Based Clinical Pathway for Parkinson’s: The vCare System Focused on Home Rehabilitation
The vCare system focuses on covering the gap in the discontinuities in institutional care available today. It aims to provide both a continuous home-based care pathway and an individualised form of virtual rehabilitation that combine Parkinson’s risk factor monitoring and physical and cognitive rehabilitation. The pathway brings together current state-of-the-art knowledge into a single clinical pathway. It also enables a high degree of personalisation of care in order to match the specific expectations and requests of patients, caregivers, and relatives.
Rehabilitation is a process by which a patient follows a care plan, firstly in a protected environment (i.e., in a clinic or a rehabilitation centre) and, secondly, at home with supervision or with the help of a clinician. Current evidence shows that home-based programmes are effective, especially in terms of patients’ capacity for exercise and health-related quality of life: they offer comparable benefits to hospital-based programmes (Parker et al. 2009; Tropea et al. 2019). Home-based rehabilitation is intended to re-build the patients’ independence and to reduce their psychological stress so that they can, once again, take part in different daily activities or re-enter the economic sphere and return to being a productive member of society (Kyriazakos et al. 2020).
Home rehabilitation with vCare has many components. It follows a clinical status monitoring routine, and includes risk prevention and motor and cognitive rehabilitation. All are synchronised by an intelligent system that interacts with the individual patient through the use of an avatar, which programmes the form of rehabilitation needed by the patient based on a plan established by clinicians. The interaction between the patient and the avatar is carried out through a television and a tablet installed in the patient’s home.
vCare rehabilitation sessions are based on a platform of video games presented on a television screen and activated by movement, which exercise motor and cognitive functions (Figure 1). The patient’s condition is monitored through different wearable sensors (a smart watch that measures heart rate and motor activity, and an accelerometer placed on a belt that checks motor status), and by his/her performance in various rehabilitation routines. The system has a series of multimedia learning or e-learning materials for risk prevention and education (this introduces the patient to risky situations associated with Parkinson’s, such as an increased risk of falls or problems with medication). The intelligent algorithms included in the vCare system adapt the rehabilitation routine established by the responsible clinicians and the e-learning routines to the patient’s own situation: they continuously inform the patient and the responsible clinician of the clinical situation and the patient’s response to rehabilitation.

Patient profiles in vCare
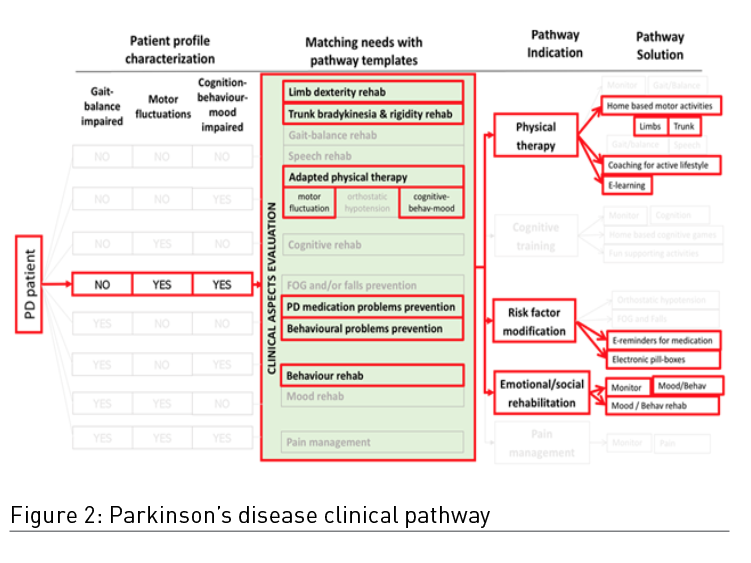
The vCare patient basic profile is based on three main criteria: Gait and balance impairment, motor fluctuations, and cognitive-behaviour-mood impairment. Once the criteria have been specified for each patient, the system adapts to matching the needs and the related pathway indications. This leads to the activation of a number of appropriate solutions. Those solutions can then be further adapted by a clinician. An example of a Parkinson’s patient profile is shown in Figure 2. The pathway combines a matching of the needs with the pathway templates, the pathway indications, and the specific pathway solution.
vCare in Practice
Once a patient has been selected for home-based rehabilitation according to appropriate inclusion/exclusion criteria, the patient is advised on how to live his or her routine life every day, with the support of a virtual coach in the form of an avatar. Interacting with the patient through a tablet, the avatar supports the patient all day long, for example, through a series of rehabilitation sessions.
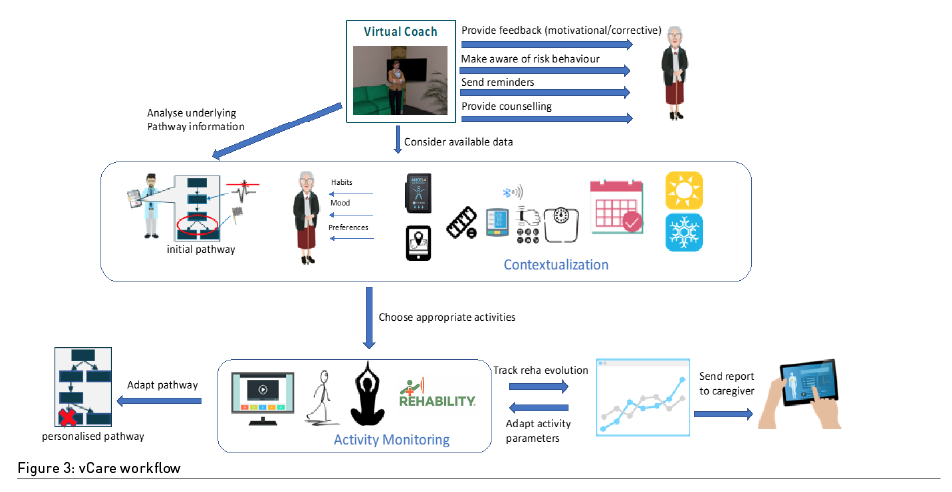
A great deal of data is involved in this whole process. Data is provided by the patients themselves, the care team, and via sensors (Figure 3). The sensors include environmental sensors to monitor movements inside the house and “motion capture” systems to evaluate the fulfilment of motor rehabilitation exercises. The data is processed continuously in order to provide appropriate advice and feedback to the patient. The clinical staff monitor the evolution of the situation on the part of the patient at any time 24/7 (i.e., during the day or night).
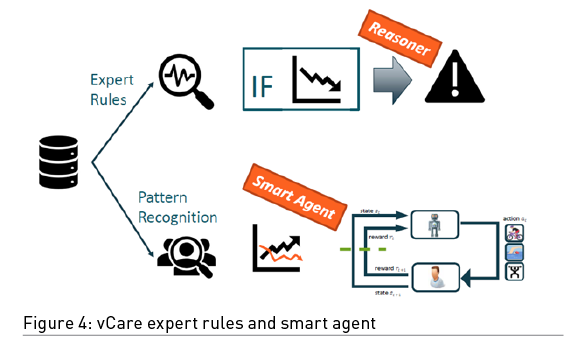
The virtual coach supplements the usual rehabilitation processes and adopts strategies that empower the patient and his/her caregiver. The personalised rehabilitation clinical pathway activated by the clinician interacts with the patient on the basis of evidence-based expert rules. It also evolves constantly in function of the patient choices and the rehabilitation goals that he or she can reach. Adaptation of the clinical pathways is ensured by embedded machine learning engines and the integration with contextual and medical information provided by sensors (Figure 4). The data is processed continuously to provide appropriate advice and feedback to the patient. The clinical staff can monitor the evolution of the patient’s situation at any time.
vCare Virtual Coach’s Range of Services
There is a wide range of interactions with the virtual coach available through the avatar displayed on the tablet. These interactions include arranging the best time schedule for the rehabilitation sessions, offering precisions and feedback about the exercises, and advising the patient about good practices to enhance his or her well-being. While the avatar can promote activities which trigger social interaction and ‘virtuous’ behaviours, it can also alert the patient when his/her behaviour is inappropriate (e.g., whenever the behaviour is too risky or the person is insufficiently active).
vCare services can be used by patients with very different conditions, which include strokes, cardiovascular conditions like ischaemic heart disease and heart failure, and neurogenerative conditions like Parkinson’s. For Parkinson’s patients in particular, vCare focuses on helping them with rehabilitation that concentrates on some specific phenomena. These include motor fluctuations, slowness of movement, posture and gait abnormalities, cognitive impairment (including memory, attention, executive function, and visuospatial abilities), fatigue, anxiety, and symptoms of depression.
Benefits to Patients and Caregivers
The benefits of vCare can be enormous. For patients: The patient is empowered to remain in control and is coached to avoid risks, such as falling, and to improve his or her own functionality, autonomy, and quality of life. For caregivers: vCare is a valuable tool that can support and educate caregivers and relatives on at least two fronts: the management of risk factors, and problem-solving in specific situations.
More specifically, the vCare virtual coaching platform aims to achieve a number of benefits/improvement for Parkinson’s patients (Table 1).
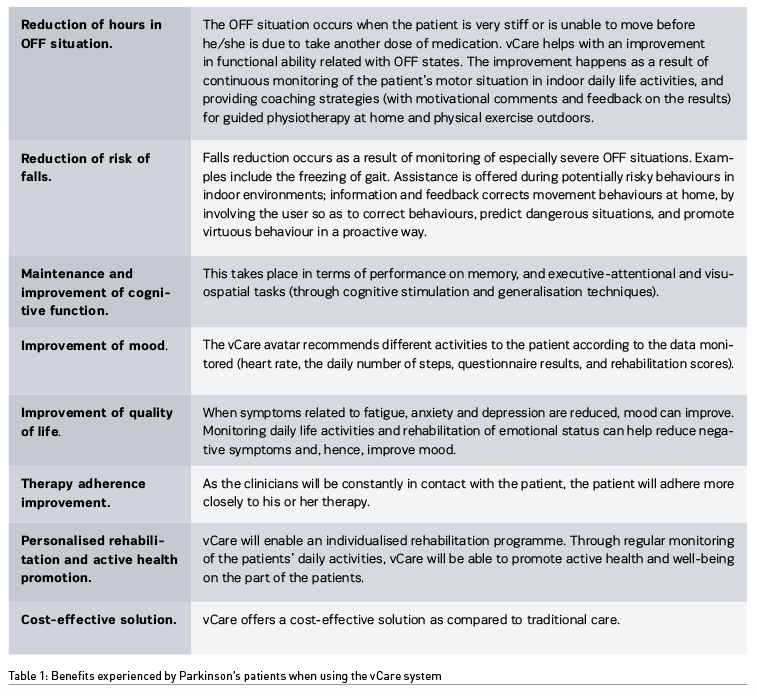
These benefits have already become evident through the work done in the Basque Country and in the vCare project as a whole.
As a next step, the vCare project team wants to collect the necessary large-scale evidence in order to convince clinicians and insurers that the solution is both effective and efficient. It will do so through a randomised control trial.
Conclusion
The vCare system is an innovative form of virtual rehabilitation. The system offers a smart solution to the currently unresolved problem of active secondary prevention for a number of pathologies. The system relies on expert evidence-based rules but also adapts to the patient’s needs and wishes through the use of machine learning. A clinical group based in the Basque Country of Spain has looked in depth at what vCare can offer to patients with Parkinson’s, especially in terms of patients’ treatment (including rehabilitation) in their own homes. Through machine learning, vCare adapts and personalises training programmes for home rehabilitation that can improve patients’ motor and non-motor symptoms and support patients’ daily life activities. As a next step, the vCare team wants to explore the collection of large-scale evidence on its benefits for Parkinson’s patients through a large, randomised control trial. Exploitation of the vCare results is ultimately expected to occur for patients with Parkinson’s.
The vCare project has received funding from the European Union’s Horizon 2020 research and innovation programme under grant agreement no. 769807.
Conflict of Interest
None.
References:
Aarsland D, BronnickK, Williams-GrayC et al. (2010) Mild cognitive impairment in Parkinson disease: A multicenter pooled analysis. Neurology. 75(12), 1062–1069.
Del PinoR, Murueta-Goyena A, Ayala U et al. (2021)Clinical long-term nocturnal sleeping disturbances and excessive daytime sleepiness in Parkinson’s disease. PLoS ONE. 16(12 December).
Emre M (2003) Dementia associated with Parkinson’s disease. Lancet Neurology.
Gómez-Esteban JC, ZarranzJJ, LezcanoE et al. (2007)Influence of motor symptoms upon the quality of life of patients with Parkinson’s disease. European Neurology.
Gómez-EstebanJC, Tijero B, SommeJ et al. (2011). Impact of psychiatric symptoms and sleep disorders on the quality of life of patients with Parkinson’s disease. Journal of Neurology. 258(3).
KyriazakosS, Schlieter H, Gand K et al. (2020) A Novel Virtual Coaching System Based on Personalized Clinical Pathways for Rehabilitation of Older Adults—Requirements and Implementation Plan of the vCare Project. Frontiers in Digital Health. 2.
ParkerSG, Oliver P, PenningtonM et al. (2009) Rehabilitation of older patients: Day hospital compared with rehabilitation at home. A randomised controlled trial. Health Technology Assessment.
Seregni A, Tricomi E, TropeaP et al. (2021) Virtual Coaching for Rehabilitation: The Participatory Design Experience of the vCare Project. Frontiers in Public Health. 9.
Somme JH, Molano SalazarA, GonzalezA et al. (2015) Cognitive and behavioral symptoms in Parkinson’s disease patients with the G2019S and R1441G mutations of the LRRK2 gene. Parkinsonism and Related Disorders.
TropeaP, Schlieter H, Sterpi I et al. (2019) Rehabilitation, the great absentee of virtual coaching in medical care: Scoping review. Journal of Medical Internet Research.
Useful websites
https://www.ehtel.eu/activities/eu-funded-projects/vcare.html




















