HealthManagement, Volume 22 - Issue 4, 2022
What is your vision of a telehealth model in the future?
During the pandemic, telehealth was a lifeline for patients who needed to consult with doctors. As many as 46% of patients used it in 2020 (Meinhardt and Staehr 2021). Some define telehealth as a combination of technology and devices used to remotely obtain information about a patient’s health status, which aids in determining whether or not an intervention is required (Galiero et al. 2020). This is how most people think of telehealth today: a patient is talking to a physician using a mobile device. Without a doubt, this is a leap forward in providing access to physician consultation. But there is more to telehealth than virtual consultations. Telehealth connects care teams and empowers caregivers to deliver care more effectively while providing the convenience that patients increasingly expect. Moreover, health systems can reduce inefficiencies and achieve growth without expanding their footprint by strategically deploying telehealth technologies throughout the patient pathway.
The current use of telehealth gives patients the ease and accessibility to obtain consultation remotely, but remote technology can considerably impact how caregivers deliver care by overcoming challenges such as geographical distance and expertise shortage posed by the traditional hub-and-spoke setups.
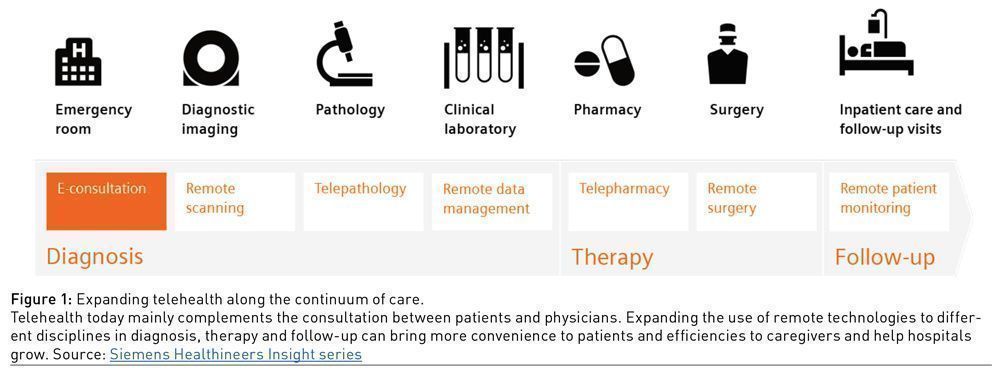
Hospitals can leverage experts across the entire network and provide patients with early diagnosis by utilising remote technologies for various disciplines. For example, with the advent of telepharmacy and remote surgery, patients no longer need to receive treatment and advanced care from specialists only on main campuses but also close to where they live and work.
Remote patient monitoring (RPM) is an important component of telehealth. What elements should be considered to optimise it?
The so-called digital front doors enable providers to remotely monitor patients’ signs and symptoms, identify when they are at risk and provide individualised care management programmes.
It all starts with engagement. Patients must be willing to contribute to the collection of data required by providers. Providers will have the data they need to provide better care if patients agree to wear wearables and other measuring and monitoring devices. Furthermore, the generated data can be aggregated and stored in an electronic health record, where patients can access, manage, and upload their health information to be shared with providers. A best practice example of this philosophy is the telehealth solution for monitoring patients with cardiovascular diseases developed by the Heart and Diabetes Center North Rhine – Westphalia (in Germany). Patients carry certified medical devices that transmit vital data to the Heart and Diabetes Center round the clock via a smartphone and a secure data connection while specialist staff at the centre collect and study data and discuss it with the patients in planned, regular phone calls, coaching and training them. This form of continuous monitoring allows for faster reaction time, guideline-oriented care and higher adherence to therapy.
What are some of the key benefits of RPM?
Remote patient monitoring is one of the most promising solutions to improve care, reduce costs and create efficiencies as it helps patients, physicians, and caregivers monitor and manage ongoing care, especially in a patient’s home. Specific applications include tablet-based patient education, videoconferencing with health care providers, and devices to prompt and track diet, exercise and medication adherence (Hodin 2017). Let me explain this with a concrete, implemented project. I’m talking about the eight years partnership Siemens Healthineers signed with the Hospital do Espírito Santo de Évora (HESE), a major hospital in the south of Portugal and the primary inpatient care facility in Alentejo, the largest region in the country. Alentejo is very rural, and the population consists largely of elderly individuals. The main cause of death is cardiovascular disease. To better respond to the needs of the local population, HESE partnered with us to implement two integrated solutions: the modernisation of the cardiac catheterisation laboratory (cath lab) and the addition of a new cath lab. Second, a telehealth programme for remote care management was developed to serve patients with cardiovascular conditions before and after interventions, such as transcatheter aortic valve implantations (TAVIs).
Remote monitoring allows hospital staff to care for patients in their homes before and after an intervention. Moreover, remote monitoring of patients in their homes has significantly improved the quality of medical care, especially in a sparsely populated region like the Alentejo, as well as made contact more personal and direct, which gives older patients in particular more confidence and security.
Although a low rate of digital literacy is a reality in the heart failure patient population, the remote care management programme encourages patient engagement and adherence, reduces hospital readmissions, and utilises artificial intelligence (AI) to streamline workflows. At home, patients have access to 24/7 support, if necessary, which improves their experience as there is no need to travel long distances for regular check-ups, and continuous care is possible despite living in different areas.
Which digital tools are essential for providing remote care?
Advances in smartphone technology, as well as healthcare provider information and communications technology infrastructure, have enabled the development of new clinical pathways involving app-based remote patient monitoring, allowing patients with chronic diseases to report on their condition from outside of the hospital, where they spend the majority of their time, putting the patient, rather than the hospital, at the centre of the care pathway. Mobile apps can provide a more valuable, real-time dataset by enabling a much faster feedback loop between patients and their care teams. In addition, remote data management technology allows laboratorians to manage increasing testing demands while providing more convenience to patients. Furthermore, with the ability for employees to view real-time data analytics and remotely access instruments for maintenance and troubleshooting, laboratory personnel can have complete oversight and control of multiple laboratories from any location. Remote patient management can also help diagnostic imaging. For example, the University of Missouri HealthCare System in the United States uses a remote scanning solution that allows medical staff to connect remotely to scanner workplaces and assist personnel in another location.
Another tool to be considered is remote robotic-assisted surgery, which can eliminate long–distance travel for patients. It also has the potential to provide greater access to patients, especially in rural areas. Robotic-supported interventions and surgical procedures do not remove humans from the care delivery process. Instead, these advancements in technology and science will improve clinical quality, patient and clinician safety, and access to lifesaving and life-extending services.
What challenges can be encountered when working on continuous real-time monitoring for patients/areas that are not connected/mobile/tech-savvy?
To effectively use digital tools and approaches in healthcare, a mindset shift and adequate training and tools are required. The digital divide must be acknowledged: not all patients own a compatible device, have adequate internet or telephone connectivity, or possess the digital skills required to use the technology.
Supporting patients through training and technical setup was beneficial during COVID-19, but new delivery models that combine face-to-face and digital services must be inclusive. And that is exactly what we did with the project in Portugal: as part of the programme, patients, families, and caregivers are educated on the remote care management solution and have access to ongoing support.
An increased level of patient engagement must be supported by resilient, high-performing supply chains. Otherwise, stock-outs or late deliveries would make these solutions meaningless and damaging to patient health. Manufacturers should consider alternative sourcing when possible. When it comes to their experiences, patients are no longer willing to differentiate between industries. As a result, patients hold hospitals to the same or similar standards to which they hold their favourite pizza chain or online retailer. As a result of the emphasis on virtual care, products and services are now being delivered to homes and locations other than hospitals. Then, hospitals must reimagine their distribution networks, including how they negotiate and collaborate with suppliers to determine the best channels to ensure the right patient receives the right products, at the right time, in the right quantity and quality (Bradley and Mangan 2021).
Do you think virtual care pathways can build patient-provider relationships as effectively as traditional care?
The basic healthcare interaction has been very human for as long as there have been doctors and nurses. This traditional human gatekeeper has served healthcare well for generations, but its limitations are becoming increasingly apparent in today’s world. Patients are increasingly approaching healthcare as consumers, expecting the same quick, convenient, easy, and affordable service they have come to expect in other aspects of their lives. In addition, the increased adoption of digital technologies like telehealth and self-monitoring devices like wearables are challenging the traditional physician-patient relationship in many ways.
A survey showed that only 36% of people under 45 now make their family doctor their first point of call for common medical issues. It is clear that patients are seeking alternative front doors (Nessim 2018).
Given this premise, the patient-provider relationship will be strengthened when digital technologies are used because patient outcomes may be better, faster, and more meaningful. At Siemens Healthineers, we believe that knowledge is power and that the more you know about your patients, the better care you can provide. e-health platforms that connect different healthcare providers, allowing them to share relevant data via teleconsultation, improve collaboration and communication across care teams and patients, resulting in better and more timely outcomes. Applications for care collaboration and patient engagement can benefit both patients and healthcare providers by facilitating interactions between care teams and their patients for timely and precise decision-making, empowering patients to actively engage in their healthcare to enable meaningful participation. One example of successful implementation of this approach is the “Online Consultation” Project” of Salzburger Landeskliniken (SALK) that is enabling virtual patient care to improve patient experience and expand access to healthcare by utilising our eHealth Virtual Visit solution that empowers patients to consult with their physicians virtually and securely from the comfort of their home and with scheduling flexibility.
Adding online consultations to the healthcare services offered by the Salzburger Landeskliniken will bring many advantages and benefits for the patients. It is much easier and more convenient for patients to make follow-up appointments. Not only will they save the time and expense of long travel and waiting times associated with an outpatient appointment, but they can also make appointments conveniently, for example, at home in their familiar surroundings. This creates a new form of proximity to the patient.
In your opinion, what are the top five challenges of monitoring patients remotely?
In my opinion, challenges could be:
- Reimbursement pathways for mobile health tools that have traditionally been a barrier to implementation.
- Healthcare providers must invest in ICT infrastructure that can rapidly translate data from apps into actionable and meaningful insights for clinicians – without becoming an additional administrative burden.
- Providers will need to invest in different skills for digital workflows, or new roles will be required within healthcare settings to support the digital patient journey.
- Confidence in these tools could be achieved with the use of digital formularies.
- Healthcare providers and developers will need to continue to work together to prioritise the standardisation of apps so that they are interoperable across health systems. As regulations differ across geographies, this will require taking into account factors including different IT architecture, connectivity requirements, and data sharing and communication standards.
RPM has a very high reliance on technology. Who bears this cost, and is this investment worth it?
Last June, Value in Health, the official journal of ISPOR—The Professional Society for Health Economics and Outcomes Research, announced the publication of a series of articles assessing the value of remote patient monitoring in addressing challenges in patient care. In the introductory editorial of the series, it is stated that “The findings from these studies suggest that RPM solutions can be cost-effective compared to usual care, although these findings may be disease-specific, context-specific, and require scale-up to achieve cost-effectiveness”. Moreover, Insider Intelligence estimates 70.6 million U.S. patients, or 26.2% of the population, will use RPM tools by 2025. And now, RPM devices are becoming smarter and more affordable (Dolan 2022).
So, it’s clear that RPM is here to stay, and healthcare providers, as well as medtech companies, should work together to create enduring value–generating partnerships to bring an innovative business model that helps provider organisation leverage technologies to upgrade their organisation both in the near term – to cope with emergencies - and in the long term, by investing in strategic digitalisation efforts. Our value partnerships approach, for instance, combines our strength in holistic medical technology management and digitalisation into a long-term performance-oriented engagement focusing on creating value. With our sustainable healthcare consulting and transformation services, as well as our future-proof design planning, we are well positioned to co-create a solution with and for our customers which will generate clinical, operational and/or financial benefits.
In your opinion, will healthcare adopt a hybrid care pathway (using both analogue and digital systems), or will the care pathway of the future be completed digitised?
Expanding the use of telehealth or remote digital technologies along the patient pathway to enable caregivers to diagnose and treat patients from another location offers the possibility of a new business model to gain greater efficiency. Moreover, the use of telehealth in patient engagement during follow-up allows caregivers to give timely, proactive care to patients for better outcomes. On the other hand, it is also quite clear that technology (i.e. Artificial Intelligence) will never replace a physician. It will be a support, making medicine more efficient, more precise and more humane. It will relieve doctors of routine work and allow them to focus on tasks AI cannot take care of: investing more time into an individual patient and making better-informed critical clinical decisions.
Disclosure of conflict of interest: Point-of-View articles are the sole opinion of the author(s) and they are part of the HealthManagement.org Corporate Engagement or Educational Community Programme.
References:
Bradley RV, Mangan B (2021) Value-based procurement: What’s in it for provider supply chains? Healthcare Purchasing News. Available from https://www.hpnonline.com/sourcing-logistics/article/21234509/valuebased-procurement-whats-in-it-for-provider-supply-chains
Case study: Outside the hospital: cancer monitoring with apps (2020). Available from https://www.siemens-healthineers.com/insights/news/case-study-cancer-monitoring-apps (produced by The Economist Intelligent Unit)
Case study: Scaling up and sustaining the digital transformation of US hospitals brought about by COVID-19 (2021). Available from https://www.siemens-healthineers.com/insights/news/case-study-us-hospitals-covid19 (produced by The Economist Intelligent Unit)
Dolan S (2022) The technology, devices, and benefits of remote patient monitoring in the healthcare industry. Insider Intelligence. Available from https://www.insiderintelligence.com/insights/remote-patient-monitoring-industry-explained/
Galiero R, Pafundi P, Nevola R et al. (2020) The importance of telemedicine during COVID-19 pandemic: a focus on diabetic retinopathy. Journal of Diabetes Research. 1-8.
Grau J, Wiegner R (2021) Redefining telehealth – driving growth through remote technologies. Siemens Healthineers Insight Series (Issue 24). Available from https://www.siemens-healthineers.com/insights/insights-series?stc=wwhc221258
Hodin M (2017) The Medical Technology That Could Save the US Billions Each Year. The Fiscal
Times. Available from https://www.thefiscaltimes.com/Columns/2017/03/03Medical-Technology-
Could-Save-US-Billions-Each-Year
Meinhardt R, Staehr H (2021) Unlocking the digital front door – How healthcare can be made more accessible. Siemens Healthineers Insights Series | The New Normal, (19). Available from https://www.siemens-healthineers.com/insights/insights-series?stc=wwhc221258
Myerson S, Thomas A, Leske M, Merges R (2022) The future of interventional services – Advancing robotics in Healthcare. Siemens Healthineers Insight Series (Issue 31). Available from https://www.siemens-healthineers.com/insights/insights-series?stc=wwhc221258
Nessim N (2018) Rise of the practical patient. Consumer healthcare report. SolvHealth. Available from https://www.solvhealth.com/for-providers/blog/2018-consumer-healthcare-report
Remote Patient Monitoring Linked to Multiple Benefits Including Cost-Effectiveness and Improved Outcomes. ISPOR. Available from https://www.newswise.com/articles/remote-patient-monitoring-linked-to-multiple-benefits-including-cost-effectiveness-and-improved-outcomes
Three supply chain opportunities for the healthcare sector. (2021) Available from https://www.consultancy.uk/news/29346/three-supply-chain-opportunities-for-the-healthcare-sector
Wiegner R (2020) This changes everything: the COVID-19 pandemic leads to a significant acceleration of digitalization in healthcare. Siemens Healthineers Insights Series | The New Normal (12). Available from https://www.siemens-healthineers.com/insights/insights-series?stc=wwhc221258
















