HealthManagement, Volume 22 - Issue 6, 2022
Key Points
- Work is where the majority of people of working age spend most of their day.
- The impact of the work environment and of workplace relationships on the individual’s psychophysical well-being has a significant and decisive influence on various aspects of their lives: their quality of life, their decision to enter (and subsequently to remain in) the working world, and the company they choose to work for.
- From the workplace to the work environment: a change in perspective is needed in order to identify what and how many factors affect the workplace well-being of people with migraine. These include the physical and social environment, collectively known as environmental factors, that, for the individual, can act as barriers or facilitators (ICF, WHO 2001).
- Inclusive safety is a passe-partout to achieve a multidisciplinary and multidimensional approach to the concept of accessibility in emergency prevention and emergency planning, an approach that considers the autonomy of every individual according to their specific needs.
Introduction
Migraine is a very complex disabling neurological disease, and currently, a large proportion of patients are only partial responders or non-responders to the available treatments. According to the WHO, migraine is the leading cause of disability in the under 50s and the second cause of years lived with disability worldwide. A recent study, in agreement with other previous studies, “revealed a high prevalence and disease burden among employees with migraine that is associated with substantial losses in productivity and employer cost” (Shimizu et al. 2021) and suggested that the development and implementation of programmes to improve migraine management in the workplace could reduce the burden and costs associated with lost workplace productivity.
The considerable social, familial, and economic impact of migraine is confirmed by epidemiological data showing that the condition occurs in 1 out of 5 women; 1 out of 16 men; 1 out of 11 children; and 1 out of 4 families. Given the marked negative impact of this disease on the quality of life and the productivity of those affected by it, its socio-economic costs are clearly very high. Unfortunately, a stigma surrounds migraine, and this has profound implications on everything concerning migraine patients, from the allocation of healthcare resources to patients’ efforts, both individual and collective, to reduce the negative impact of the disease (Parikh and Young 2019). Understanding the stigma of migraine and learning how to develop effective ways to mitigate it can increase the quality of life of these patients. The Alliance for Headache Disorders Advocacy, for example, has sought to address the structural stigma inherent in discriminatory policies of employers, government agencies, and public institutions. Such efforts can help considerably to improve the conditions of these patients (Shapiro 2020), as well as reduce the negative impact of workplaces that fail to meet their needs.
On 14 July 2020, in Italy, an important law concerning primary chronic headache was passed. Law 81/2020 recognises headache as a social disease. It represents a fundamental step towards having clear, certain, and well-defined regulatory references and a system designed to guarantee the patient prompt entry into the healthcare system, a correct diagnosis, and adequate therapies.
Recognition of migraine as a social disease, however, does not automatically imply its recognition as a disabling disease. For many migraine sufferers today, being recognised as a person with disability seems to be the only way they can legitimise their status as “sick people” in workplaces that they continue to find absolutely inadequate for the needs of people with invisible diseases.
In an economic and social context in which companies are increasingly building their policies around the concepts of social sustainability and employee well-being, it has become necessary to rethink the workplace in such a way as to make it more inclusive for those suffering from diseases that cause temporary, permanent or dynamic disability. We need to rethink the workplace in terms of a work environment that is expressed in several dimensions: spatial, organisational, and relational.
This goal can be achieved only if the accommodations made stem from an awareness of the extent to which the environment can be a facilitator or an obstacle in our daily lives.
Gaining this awareness demands a change in perspective. The workplace has to stop being a place you need to escape from when you are sick, an environment full of triggers, where migraine is a taboo subject and those affected by the condition are stigmatised as “shirkers”.
We need to rethink the work environment in terms of making it a welcoming and safe place that helps people with migraine to manage their disease and, as such, provides them with additional support alongside the drug therapies and other non-pharmacological strategies that can help them to manage their disease and feel better.
What effects would a change of this kind have?
- Reduced presenteeism and absenteeism and increased productivity.
- Reduced social costs of migraine.
- Reduced impact of the disease on the lives of those who have it.
- Reduced impact of the disease on social relations at work.
The Workplace as a Facilitator
Work is where the majority of people of working age spend most of their day. Attention to the well-being and safety of people in the workplace is therefore crucial not only to their experience of both the work and the place but also to their whole quality of life.
Companies and organisations, in general, are becoming more and more oriented towards discovering, embracing, and managing diversity, a trend that sees them valuing the uniqueness of people through the application of a philosophy of inclusivity in different areas: communication and attitudes, organisation and procedures, environmental planning, and safety.
Diversity and inclusion are the focus of the “ISO 30415:2021 - Human Resources Management - Diversity and Inclusion” standard, a reference document that helps those organisations that value diversity as an essential condition for business growth and greater efficiency and competitiveness to integrate this principle into their management systems. Its aim is to help organisations to develop inclusive workplaces by addressing inequalities in their systems, policies, processes, and practices, as well as in people’s conscious and unconscious biases and behaviours.
It is important to consider that workplaces are not frequented exclusively by workers, but also by occasional or regular visitors (e.g., customers, users, maintenance technicians, etc.), who may spend anything from minutes or hours to whole days, or longer, there. In fact, workplaces include schools, health facilities, places of cultural interest, hospitality facilities, commercial establishments, sports facilities, public entertainment venues, and all production facilities and public offices. Many of these places, such as cinemas and shopping malls, are crowded, and some activities are carried out in open spaces.
Although these places differ structurally and in terms of their spaces, fittings and functions, as well as the people who use them, they all seem to be designed with more attention to the “container” and its intended use than to the performance levels determined by the interaction between the environment and people.
In other words, the aspect that most designs seem to neglect is precisely the human component: people and their different needs and abilities. Or, at best, they employ models that do not really reflect human variability and its nuances and are thus based on a representation of this component that does not correspond to reality.
It is important to promote awareness of how an environment can hinder or facilitate the autonomy in ordinary situations of each person in it, not to mention individual performances, and thus the collective response, in emergencies (Schiavone 2021).
In the International Classification of Functioning, Disability and Health (ICF), disability is conceived as an umbrella term covering impairments, activity limitations, and participation restrictions. It denotes the negative aspects of the interaction between a person’s health condition(s) and that same individual’s contextual factors (environmental and personal factors).
Unfavourable environmental conditions with respect to individual health conditions can indeed cause disability (albeit not certifiable disability) or, in any case, limit autonomy and generate discomfort and malaise.
One example of how context can represent a barrier for many, or sometimes al people is that of an emergency situation, where the effects of some major event, be it a fire, earthquake, flood or other, change the whole scenario, with the result that the services provided in ordinary circumstances are no longer guaranteed or adequate.
This example underlines the importance of designing workplaces according to the criteria of inclusive safety and of including, in the emergency prevention and management system, solutions that also enable people with disabilities to respond independently to emergency situations. Or in any case, solutions that envisage adequate training of operators and rescuers take into account the possibility of needing to help or rescue people according to their specific individual needs (Zanut and Schiavone 2021).
There are several ways to help support people with migraine in the workplace and increase their productivity. These include workplace migraine education and management programmes, the creation of migraine-friendly work environments, migraine treatment optimisation, and advocacy (Dodick et al. 2018). Adapting the workplace to patients’ needs could also significantly improve their condition.
Below we examine several elements that can improve the performance of the environment vis-à-vis people who suffer from migraine and represent facilitators for those with other disabilities too.
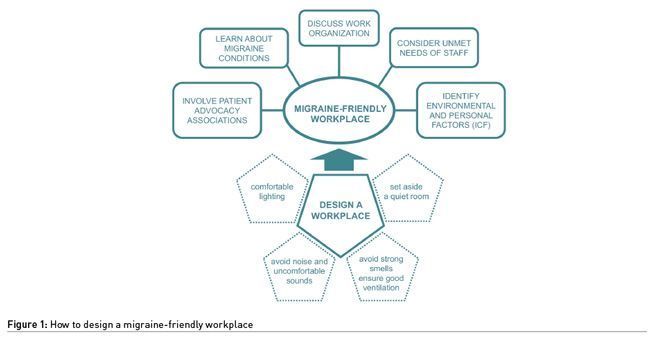
Designing a Workplace That Considers the Needs of People With Migraine
In research conducted by the University of Rochester School of Medicine and Dentistry (Rochester, NY), the following emerged: “Migraineurs often describe environmental triggers of their headaches, such as barometric pressure change, bright sunlight, flickering lights, air quality, and odours. Environmental aspects of indoor spaces and workplaces are also implicated in migraine experiences. Comprehensive migraine treatment programmes emphasise awareness and avoidance of trigger factors as part of the therapeutic regimen” (Friedman and De Ver Dye 2009).
In light of new knowledge, efforts to improve the workplace user experience, for workers generally and for those with migraine, in particular, should focus more on the correlation between trigger factors and symptoms, both to prevent headache attacks and also to facilitate recovery from them.
Below we provide a concise (and therefore not exhaustive) overview of migraine symptoms and possible measures, useful for creating a more inclusive and accessible environment for people with this and also certain other conditions.
Photophobia: hypersensitivity to light
- Who has this sensitivity? It occurs in more than 80% of people with migraine and can also be found in neurological diseases such as multiple sclerosis (MS), autism spectrum disorders, eye diseases, and as a side effect of some drugs;
- What does it entail? It can cause migraine in predisposed subjects, but also discomfort and ocular pain;
- What are its environmental triggers? Sunlight and artificial light.
Environmental facilitators to prevent and reduce the impact of photophobia:
- Use shading systems for windows and glass walls that make it possible to adjust the intensity and direction of natural light;
- Use artificial lighting systems that allow the environment to be adapted to specific situations, work phases, or users’ temporary needs;
- Avoid lighting fixtures in which the light source is directly visible;
- Opt for indirect lighting;
- Equip workstations with adjustable lighting systems (adjustable direction, luminance, and light temperature);
- Avoid reflective surfaces.
Phonophobia: an aversion to sounds that are normally tolerated, i.e., normal ambient sounds
- Who has this sensitivity? This symptom is found in 70-80% of migraine patients during an acute attack; in general, people with sensory hypersensitivity can also experience these symptoms, including people on the autism spectrum and people with hyperacusis, misophonia, tinnitus, or neurodegenerative conditions such as MS;
- What does it entail? It can cause migraine in those who suffer from the condition; sensory stimulation can be a cause of meltdown in autistic subjects.
- What are its environmental triggers? Sounds, music, and noises whose frequency and volume are not tolerated (tolerability is subjective), such as the sounds of traffic, dishes, loud conversations, sirens, and alarms.
Environmental facilitators to prevent and reduce the impact of phonophobia:
- Avoid creating environments liable to generate echoes and reverberations;
- Avoid bells, ringtones, and loud music;
- Avoid loud alarms, sirens, and voice messages;
- Adopt noise mitigation measures (e.g., sound-absorbing panels and furnishings) in large, highly crowded environments and wherever else they are considered necessary.
Osmophobia: increased sensitivity and intolerance to some smells
This is subjective and varies from individual to individual. In some predisposed subjects, strong smells are a migraine trigger, while in others, sensitivity and intolerance increase during headache attacks.
- Who has this sensitivity? It affects 84% of patients suffering from migraine with aura, 74% of those affected by migraine without aura, and 43.3% of those with tension-type headaches. It can also occur in some psychiatric disorders, in pregnant women, and in people whose sense of smell is affected by the drugs they are taking.
- What does it entail? It can cause migraine (in migraine sufferers), nausea, and vomiting;
- What are its environmental triggers? The most offensive smells are strong perfumes, food smells, and cigarette smoke.
Environmental facilitators to prevent and reduce the impact of osmophobia:
- Avoid perfume diffusers;
- Choose odourless cleaners and disinfectants;
- Use extractors in kitchens and wherever processes are being carried out that involve the use of solvents, paints, or other materials with smells/perfumes that can trouble the most sensitive people;
- Ensure good air exchange through natural ventilation;
- Use air purification systems where necessary.
Given the subjective nature of migraine symptoms, triggers, and intensity, in addition to taking all the basic precautions to ensure the well-being of workers, it is always advisable to share with them any decisions on specific environmental measures to be implemented.
The various environmental facilitators listed are all expedients that, if duly considered in the design phase, together with any solutions necessary for customising the environment, can easily be regulated during the use of the building.
A design approach that takes into account the variability of human needs will improve the quality of the environment as a whole, guaranteeing full accessibility and safety of spaces, equipment, and services for everyone. Involving workers in the sharing of needs and related choices is essential for the creation of an inclusive workplace. In the context of efforts to meet the needs of people with migraine, this approach should be extended, beyond issues concerning the physical space, to a discussion of the organisation of work and of individual behaviours that can act as triggers, such as wearing perfume or smoking cigarettes, including e-cigarettes.
It is essential that teams designing work environments include technicians with expertise in accessibility, lighting, and acoustics so as to guarantee the creation of environments capable of responding and adapting to the specific needs of people and contexts.
In addition to working on elements capable of reducing the risk of the onset of symptoms and of mitigating their impact, it is useful to provide, where possible, an environment where people affected by migraine can isolate and recover.
A quiet room can be appreciated not only by people with migraines but also by those with autism spectrum disorders recovering from a meltdown, by those with MS fatigue, or with other specific needs. Soft furnishings where people can lie down, low saturation colours, plants, and colour-adjustable lights are some of the measures that can be adopted in the quiet room. The design of the emergency prevention and management system, including the orientation and wayfinding system, the emergency devices, the alarm system, and the escape routes, must also take into account the specific needs described above since a stressful situation, like an emergency, can trigger an attack and consequently impair the individual’s ability to adequately respond (Schiavone 2022).
Conflict of Interest
None.
References:
Dodick D, Edvinsson L, Makino T et al. (2018) Vancouver Declaration on Global Headache Patient Advocacy 2018. Cephalalgia. 38(13):1899-1909.
Friedman DI, De Ver Dye T (2009) Migraine and the Environment. Headache The Journal of Head and Face Pain. 49(6):941-952.
Parikh SK, Young WB (2019) Migraine: stigma in society. Curr Pain Headache Rep. 23(1):8.
Schiavone E (2022) Progettare la sicurezza inclusiva: da dove iniziare? in PdE, Rivista di psicologia applicata all’emergenza, alla sicurezza e all’ambiente, Anno 19, numero 63, Giugno 2022, ISSN 2531-4157 (p. 7/10).
Schiavone E (2021) Dalla sicurezza dei luoghi alla sicurezza delle persone, in PdE, Rivista di psicologia applicata all’emergenza, alla sicurezza e all’ambiente, Anno 18, numero 60, Ottobre 2021, ISSN 2531-4157 (p. 7/10).
Shapiro RE (2020) What will it take to move the needle for headache disorders? An advocacy perspective. Headache. (9):2059-2077.
Shimizu T, Sakai F, Miyake H et al. (2021) Disability, quality of life, productivity impairment and employer costs of migraine in the workplace. J Headache Pain. 22(1):29.
Zanut S, Schiavone E (2021) Persone reali e sicurezza inclusiva. Il contributo della progettazione inclusiva alla sicurezza di tutti, in ANTINCENDIO n.1/2021(p. 56/71), EPC Editore.




















