HealthManagement, Volume 3 - Issue 1, 2009
Clinical trials measure healthcare outcomes to determine the efficacy of healthcare interventions. Economic evaluations provide valuable information to help decision- makers allocate scarce resources more efficiently and to see whether the intervention represents good value for money. Two methods can be used to determine cost-effectiveness: an economic evaluation alongside a clinical trial, which estimates the costs and outcomes during the trial period; and a modelling approach extrapolating costs beyond the trial duration. This article will describe what an economic evaluation is and how to conduct one.
What is Economic Evaluation?
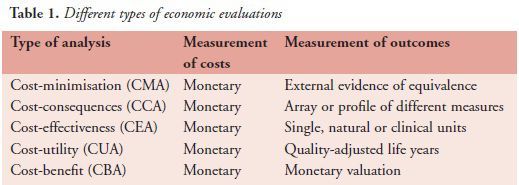
Economic evaluation is concerned with minimising opportunity costs (the value of the next best alternative foregone as a result of the decision made) so that the best use is made of scarce resources. Therefore, we have to make choices, by comparing costs and outcomes of alternative treatments. The basic tasks of any economic evaluation are to identify, measure, value and compare the costs and consequences of the alternatives being considered. There are five types of economic evaluation (see table 1) and each measures costs in monetary units. However, they differ in the way consequences are included.
At the start of any economic evaluation, you need to specify the following:
- Research question (i.e. the cost effectiveness of cardiac interventions);
- Study perspective (i.e. healthcare);
- Time frame of analysis (i.e. lifetime of patients);
- Analytical approach (i.e. decision model);
- Options for comparison (i.e. drug A compared with drug B), and
- Approach to costs and outcomes (see fig. 1).
Each of these issues will determine the scope of costs and
outcomes; which are included, how they are measured and valued, and how they
are reported and interpreted.
Determine Which Costs are Relevant
The study perspective will determine which costs are considered
relevant for the evaluation. For any economic evaluation, you need to identify
categories of key resource use (i.e. inpatient stays) and then measure them in
their physical units (i.e. number of bed days). There are various sources that
we can use to measure resource use, such as randomised trials, clinical
databases, medical records, patient questionnaires and literature. Ideally for any
economic evaluation, resources should be valued by their opportunity cost.
However, this is not always practical and market prices are usually used to value resources in units of local currency (i.e. average cost per
bed day).
Valuing Health Outcomes
The outcomes used in economic evaluations depend on the research question and the type of evaluation being conducted (see table 1). These include:
- Clinical measures which use natural units (i.e. number of cardiac cases detected);
- Disease specific instruments (i.e. hospital anxiety and depression scale);
- Mortality measures which look at life years gained;
- Generic measures which use instruments to measure overall health related quality of life (HRQQL), etc.);
- Utility measures, a special kind of generic measure that give an indication of value placed upon the HRQOL (i.e. EQ-5D), and
- Monetary measures which value benefits in terms of currency.
There are two main approaches to valuing health outcomes: monetary
and nonmonetary. Non-monetary valuations include scales that ask participants
to rank health outcomes or place outcomes on a scale such as the visual
analogue scale. Also, the standard gamble approach is based on the axioms of
expected utility theory and asks respondents to make choices that weigh
improvements in health against mortality risks. Finally there is the time
trade-off approach, a method for valuing health states that asks respondents to
make hypothetical choices that weigh improvements in health against reduced
longevity. Monetary valuations include revealed preferences where individuals
assess the benefits in accordance with their preferences; and stated preferences
are where valuations are derived from surveys such as willingnessto- pay
studies.
The Role of “Modelling” in Evaluation
Modelling is used in economic evaluations when trial data does not exist, and can be used to extrapolate existing data beyond a certain time period. Decision analytical modelling represents the various clinical pathways for alternative treatments and quantifies the probability of a patient following each pathway. For each pathway, the range of possible costs and health-related outcomes can be calculated.
The aim of the decision model is to calculate the expected (i.e. the mean) costs and outcomes of the alternatives together with the uncertainty in those estimates. Decision modelling looks at a process in which a fixed sequence of events leads to an outcome, but does not take into account the time dimension. On the other hand, Markov modelling is useful in analysing the evolution of health states over time for a particular illness.
Handling Uncertainty
Every economic evaluation will contain some degree of uncertainty: parameter uncertainty is where you are unsure about the true numerical values of the parameters used as inputs; and model uncertainty is where you are unsure about the correct method for combining parameters, and/or the analysis which may have been completed. There are several methods for handling uncertainty, the simplest being a one-way sensitivity analysis, where each parameter is varied one at a time in order to investigate the impact on study results, through to more sophisticated methods such as probabilistic sensitivity analysis where one can incorporate the uncertainty of all the parameters in the model simultaneously.
Presentation and Interpretation of Results
If the study period in question is greater than a year, then costs
and outcomes should be discounted. Discounting allows future costs to be
converted into present values, thereby allowing comparisons between costs and
outcomes that occur at different times. The incremental cost-effectiveness ratio
(ICER) is the difference in costs between one intervention and an alternative, divided
by the difference in outcomes. This ratio represents the extra amount one would
pay for an additional unit of health outcome. Cost-effectiveness planes are
used to present results (see fig. 1).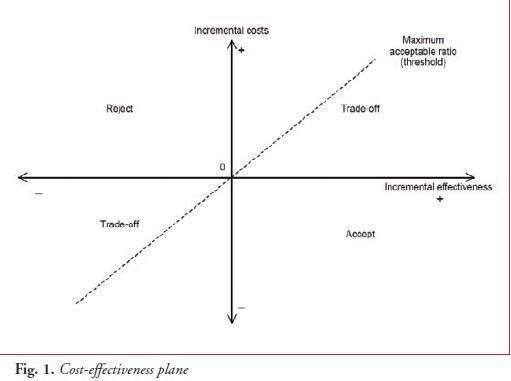
In this figure, the x axis represents the differences in effects for two interventions and the y axis represents the difference in costs for the two interventions. The slope of the line is known as the maximum acceptable ICER. If the costs and benefits for the intervention fall below that threshold you would probably choose to adopt it. The uncertainty in economic evaluations are presented as cost-effectiveness acceptability curves (CEACs) which are used to indicate the probability that an intervention is more cost-effective than the alternative for a range of potential maximum amounts (ceiling ratio) that a decision-maker is willing to pay.
Conclusions
Economic evaluations are increasingly being used to inform decision-making about which healthcare interventions should be used adopted. For any economic evaluation, the following need to be considered: the research question, the study perspective, the time horizon, the analytical approach, the options for comparison, the approach to costs and outcomes and dealing with uncertainty.



















